
A letter from Tamera Dunseth Rosenbaum
I am honored to serve as Chief Nursing Executive for UCHealth and Chief Nursing Officer for the UCHealth Southern Colorado Region. Across 14 hospitals and more than 250 clinics, our teams of more than 11,500 UCHealth nurses support patients and families in collaboration with our interdisciplinary colleagues. I am committed to live our mission by improving the lives of not only our patients, but our clinical teams as well.
Our culture empowers nurses as advocates dedicated to elevating the quality of care. They are partners and key strategists who pursue life-long learning, who teach and collaborate across the organization. Opportunities such as the UCHealth Ascend Career Program, UEXCEL program and mentoring support our nurses through career advancement and development.
At UCHealth, we adhere to evidence-based practices and continually evaluate outcomes. We value patients first, and their safety is top priority. In addition to robust training, policies and protocols, we have deployed leading-edge technology to support bedside staff. The UCHealth Virtual Health Center (VHC) is a 24/7 operation supporting our hospitals to monitor patient conditions, prevent falls, detect early signs of sepsis and deterioration, and more. Further, our innovative models of care strategically place resources to best support our teams and enable nurses to perform at top-of-scope.
UCHealth nurses maintain a genuine focus on our patients and their families. They advance their expertise as leaders in unrelenting pursuit of excellence to improve lives.
Tamera Dunseth Rosenbaum DNP, RN, NE-BC
Your nursing career at UCHealth
Make Extraordinary Possible.
At UCHealth, we’re looking for professionals who are talented, inspired and eager to meet challenges.
For those individuals called to join our award-winning nursing staff, we want you to find more than just a career here. We want you to make extraordinary possible.
UCHealth Nursing Professional Practice Model

Nursing at UCHealth hospitals
Broomfield Hospital

Contributions of Professional Nursing
- Erin Brix, BSN, RN, Charge Nurse – Preoperative/PACU. Erin identified an opportunity to improve practices and reduce costs for the entire UCHealth system while improving the preoperative nasal decolonization swab process used to prevent surgical site infections (SSI). Not only is the new swab and process more comfortable for patients, it has provided cost savings of approximately $100,000 for all of UCHealth.
- Sarah Fahs, RN, Charge Nurse – Medical Surgical Unit. Sarah consistently demonstrates high work ethics and standards. She is a steadfast nurse, solidly committed to the best quality outcomes of all of the patients on the Medical Surgical Unit.
Grandview Hospital
Director of Nursing: Courtney Hoffbauer, DNP, RN-BC, NE-BC
Hospital Recognition
- Joint Commission Disease Specific Total Hip & Knee Replacement
- DNV Accreditation: Stroke-Ready Hospital
Contributions of Professional Nursing
- Implementation of Robotically-Assisted Orthopedic Surgery Partial & Total Knee Mako program.
- Jessica Clute BSN, RN-ONC, Inpatient Unit Nurse Manager & Carol Mantilla BSN, RN-ONC, Orthopedic Nurse Navigator. Presentation accepted at National Association for Orthopedic Nursing Conference: Enhancing patient knowledge: A standardized discharge class for total joint replacement (May 22-25, 2021).
- Nicole Harding, MSN, RN – Case Management. As a case manager who supports long-term placement patients, Nicole was recognized for consistently helping her unit colleagues by working clinical nursing shifts on the floor, including night shifts.
Greeley Hospital

Hospital Recognition
- Level III Trauma Center re-designation 2024
- Lown Institute Hospitals Index #2 in the nation and #1 in the state, 2023-2024
- Geriatric Emergency Department Accreditation 2023
- Institute for Healthcare Improvement (IHI) Participant Age Friendly Health System Participant since 2023
- Re-accredited with the Joint Commission 2023
- 4-star rating from CMS, 2023
- First place in Healthcare Innovator Awards program, 2021

American Nurses Credentialing Center (ANCC) Pathway to Excellence® designated: 2024.
Contributions of Professional Nursing
- Angel Armamento, Birthing Center / 2026 Pathway Direct Care Nurse Award: Quality. Angel is a Birthing Center nurse whose authentic, approachable leadership consistently elevates patient care and team performance. She ensures every patient feels heard, respected, and supported, creating an environment where questions, concerns, and shared decision-making are welcomed. Angel has led impactful quality improvement efforts, including development of an Empowerment Cart that supports physiologic birth, enhances RN confidence with movement, positioning, and nonpharmacologic pain management, and promotes evidence-based practice. She also implemented an OR hemorrhage case cart, improving efficiency, response time, and coordination during high-risk events, directly strengthening maternal safety. Committed to continuous improvement, Angel actively seeks team feedback and applies data through Unit-Based Council work, notably driving a pain reassessment documentation initiative that achieved a 10% improvement this fiscal year toward exceeding 90% compliance. She is deeply dedicated to education, serving as a preceptor, mentor, and supporter of peers and learners. She consistently turns ideas into action and improves outcomes.
- Seth Henkel, PCU / 2026 Pathway Non-Direct Care Nurse Award: Leadership. Seth exemplifies Pathway-aligned nursing leadership through consistent engagement, transparency, accountability, and staff empowerment. His people-centered approach produced improvements in culture and outcomes, evidenced by Employee Voice Survey gains between February and October 2025: Engagement Index rose from 56.1% to 87.5%, favorable feedback on individual performance reached 100%, and staff involvement in decision-making more than doubled. These results reflect Seth’s sustainable strategies. He built a cohesive, high-performing charge nurse team with clear roles and aligned priorities, improving workflow reliability. Through structured listening sessions and consistent follow-through, he strengthened trust and shared governance. Transparency is reinforced via a unit-based stoplight report that promotes open communication, shared accountability, and proactive problem-solving. Seth invests in individualized leadership through regular one-on-one coaching and tailored professional development. He also champions staff safety through workplace violence initiatives and co-led implementation of a two-tier patient escalation pathway at Greeley Hospital, improving response times, staff confidence, and patient management.
Highlands Ranch Hospital

MS, RN
Hospital Recognition
- The Joint Commission’s Certificate of Distinction for Primary Stroke Centers.
- Inpatient epilepsy monitoring unit led by neurologists who are board certified in neurology and epilepsy to help diagnose and construct the best treatment plans.
- Level III Trauma Center.
Contributions of Professional Nursing
- Melody Stendahl, BSN, RN, Clinical Nurse – ICU / DAISY Award winner. Melody received the DAISY Award for her extraordinary care of a patient who required intubation. The patient had recently lost her mother and stated that Melody’s reassuring presence helped her feel safe and supported during this difficult time.
- Megan Reffel, BSN, RNC-NIC, CLC, Charge Nurse – NICU. Megan was recognized in the 1st Annual UCHealth Nursing Research Fellowship Completion Ceremony on June 9, 2021 for her research work titled “Nurse Perceptions of Neonatal Collapse on Postpartum Units.”
Longs Peak Hospital

Hospital Recognition

American Nurses Credentialing Center (ANCC) Pathway to Excellence® designated: 2024.
- AHA Primary Stroke Certified 2018.
- ACEP Accredited Geriatric Emergency Department 2018.
- Level III trauma center 2017.
- Low Acuity Bariatric Center of Excellence 2021.
Contributions of Professional Nursing
- Elizabeth Smith, Medical Oncology Unit / 2026 Pathway Direct Care Nurse Award: Quality. In her charge nurse role, Elizabeth drives measurable, sustained quality outcomes within a high acuity oncology setting by blending hands on clinical care with strong unit level leadership. She led development and implementation of a Turn Team model when every two hour repositioning compliance averaged nearly 50%. By standardizing Braden scoring accuracy, clarifying expectations, strengthening real time documentation, and defining accountability, compliance improved to greater than 80% and has remained sustained, significantly reducing pressure injury risk. Recognizing mobility as a key outcome driver, Elizabeth implemented mid shift mobility goal check ins, resulting in the Medical Oncology unit at Longs Peak Hospital becoming a top system performer for mobility goal achievement. She also independently created a Charge Guided Audit Tool, improving documentation reliability, continuity of care, and shared accountability. An oncology trained nurse nearing completion of her Nurse Practitioner program, Elizabeth consistently applies advanced clinical judgment to support safe, evidence based care and exemplifies the Pathway Quality standard.
- Geoffrey Bradbury, Medical Surgical Progressive Care Unit / 2026 Pathway Non-Direct Care Nurse: Professional Development. Geoffrey is a Clinical Nurse Educator for the Medical Surgical and Medical Oncology units at Longs Peak Hospital whose leadership and innovation have elevated nursing excellence and professional development. He ensures equitable access to education by supporting staff across all shifts, strengthening confidence, engagement, and retention—especially among new graduates through Starry Night education and six month check ins. Geoff’s data driven initiatives have closed critical knowledge gaps, including development of a Total Hip and Knee Scavenger Hunt and Ortho Bootcamp, achieving over 65% staff engagement and improved orthopedic competency. He implemented hands on heparin education, increasing participation by at least 30% and enhancing medication safety, and introduced in person Lap/Roll belt training, resulting in a 100% reduction in falls with injury related to missing belts. He also leads Everybody Moves mobility education. In collaboration with Medical Oncology Unit Based Council, Geoff advanced chemotherapy certification, with 86% of staff certified or in progress, directly improving patient safety and the practice environment.
- Jenifer James, BSN, RN, IBCLC, Registered Nurse, Birth Center / 2020 DAISY Award. Jenifer was recognized for the extraordinary care she gives laboring and postpartum patients by creating a unique and meaningful birth experience for them. Jenifer builds relationships with her patients and their families to learn what is important to them and incorporates their needs into their care.
- Jeanine Snyder, BSN, RN, CCRN, Registered Nurse, Post-Anesthesia Care Unit / 2021 Colorado Hospital Super Hero Award. With a strong background in critical care nursing, Jeanine stepped up to assist the hospital intensive care unit caring for the hospital’s sickest patients. She quickly became a reliable clinical resource among the group and an extraordinary colleague.
2024 DAISY Awardees
- Joe Tempel, Acute Care: received the DAISY award for prompt, knowledgeable care and extraordinary pain management.
- Eugene Collins, Medical/Oncology: received the DAISY award for professionalism, responsiveness, compassion and caring.
- Taylor Nolte, Birth Center: received the DAISY award for kindness, caring, and physical and emotional support.
- Chris Withbroe, DAISY Nurse Leader awardee for embracing the UCHealth mission and values in all that she does.
Medical Center of the Rockies

RN, CENP
Hospital Recognition
American Nurses Credentialing Center (ANCC) Magnet® designated: 2010, 2016, 2021, 2025.

- Colorado Department of Public Health and Environment Level I Trauma Center 2022
- American College of Surgeons (ACS) Level I Trauma Center 2023
- Advanced Certification as a Primary Stroke Center by The Joint Commission in 2021 and 2023
- American Heart Association/American Stroke Association Certification as Primary Stroke Center in 2021 and 2023
- American Heart Association/American Stroke Association Get with The Guidelines Stroke Gold Plus Quality Award with Honor Roll Elite Plus in 2021, 2022 and 2023
- Cardiac Surgery Unit Advanced Life Support (CSU-ALS) Center of Excellence
- Get with the Guidelines STEMI Receiving Center
- American Heart Association Get with the Guidelines Heart Failure Gold Plus with Target: Heart Failure Honor Roll and Target: Type 2 Diabetes Honor Roll in 2024
- Institute for Healthcare Improvement (IHI) Participant Age-Friendly Health Systems Participant since 2020
- US News & World Report #2 hospital in Colorado in 2022, 2023, and 2024
- Lown Institute Hospitals Index #4 most socially responsible hospital in the United States and #2 in Colorado in 2023
Contributions of Professional Nursing
- Elisabeth Elsner – Medical Unit / 2026 Magnet Nurse Award for Transformational Leadership. Elisabeth exemplifies Transformational Leadership through her ability to empower others, strengthen unit culture, and inspire excellence during times of change. As a charge nurse, she provides steady, trusted leadership on night shift, fostering confidence, cohesion, and psychological safety while supporting staff through ongoing challenges.
Elisabeth is deeply committed to developing others. Over the past year, she has supported the onboarding and growth of many new staff. She intentionally works alongside new relief charge nurses during high-acuity situations, offering real-time coaching in prioritization, decision-making, and de-escalation. Staff frequently describe her as approachable and supportive, noting that she helps them gain confidence and succeed in their roles.
Her hands-on leadership directly supports patient safety and clinical excellence. Through consistent reinforcement of best practices and real-time oversight, the unit has maintained zero CLABSIs for two consecutive years, zero CAUTIs for 18 months, and 98% falls bundle compliance.
Despite staffing challenges and rapid onboarding, morale remains strong. Elisabeth’s steady, inspiring leadership continues to positively shape people, outcomes, and culture. - Ryley DeLuca – Surgical PCU / 2026 Magnet Nurse Award for Structural Empowerment. Ryley is a clinical leader whose commitment to shared leadership, professional development, and lifelong learning has led to meaningful and lasting improvements on the Surgical Progressive Care Unit. As a trusted night-shift charge nurse and preceptor, she actively participates in shared governance through the Unit-Based Council, advocating for bedside nurses and addressing pediatric-specific needs in a mixed-acuity environment.
As the unit’s pediatric champion, Ryley led the development and implementation of key pediatric resources, including updates to the pediatric crash cart, PEWS tools, vital sign charts, and a pediatric admission checklist. These tools have improved standardization, confidence, and safety in pediatric care. She further promotes professional growth by teaching monthly Tiny Steps pediatric education classes and creating concise, evidence-based tip sheets used in orientation and daily handovers.
Currently pursuing Level III in the UEXCEL program, Ryley leads a pediatric quality initiative and has precepted five new nurses. Her work resulted in a 79% increase in pediatric education attendance and strengthened unit readiness. - Livvy Armstrong – Surgical ICU / 2026 Magnet Nurse Award for Exemplary Professional Practice. Since joining the SICU as a new graduate nurse in July 2024, Livvy has demonstrated exceptional clinical growth, professionalism, and compassion in a demanding high‑acuity environment. She has approached the transition into critical care with resilience, humility, and a strong commitment to learning, quickly developing clinical competence and situational awareness beyond her experience level. Livvy consistently advocates for her patients while remaining a reliable and supportive team member.
Her impact is deeply reflected in patient and family experiences. Families describe her calm confidence, compassion, and steady presence during vulnerable moments, with one patient stating she provided “the best care I’ve ever received in the hospital.” Livvy intuitively meets both patient and family needs, frequently going above and beyond.
Livvy is also dedicated to lifelong learning and knowledge sharing, seeking the “why” behind care decisions and clearly supporting peers during high‑acuity situations. She exemplifies teamwork, accountability, and Magnet principles, making her highly deserving of Magnet Nurse recognition. - Amelia Molina – Clinical Quality / 2026 Magnet Nurse Award for New Knowledge, Innovations, and Improvements. Amelia is a highly effective Clinical Quality and Safety Specialist whose work has significantly advanced outcomes for patients with cardiogenic shock across the Cardiovascular Service Line. Through regional mortality reviews, she identified delays in diagnosis and treatment and partnered with physician leaders and multidisciplinary teams to design and implement a Cardiogenic Shock Team in under one year. Her leadership supported development of clear clinical algorithms, performance metrics, order panels, EHR workflows, and IT alerts, resulting in improved early recognition and coordinated response across the North Region.
Amelia further established a Cardiogenic Shock Case Review Committee to drive continuous improvement, inform education, and guide system enhancements such as a SCAI shock calculator and expanded Agile Pathways. She leads ongoing interdisciplinary education for nurses and providers, contributing to statistically significant improvements in observed-to-expected cardiology mortality in 2025. Through innovation, analytics, education, and collaboration—including a cardiogenic shock survivor group—Amelia exemplifies Magnet nursing and system-level clinical leadership. - April Hettinger – Admit/Discharge / 2026 Magnet Nurse Award for Empirical Outcomes. April exemplifies nursing excellence through her measurable impact on patient outcomes, staff engagement, and unit safety culture as the MCR Medical Unit’s dedicated Patient Flow RN. Her leadership and commitment to patient‑centered care strongly reflect Magnet principles. A key accomplishment has been her leadership in improving patient mobility. At the start of 2025, the unit’s “Mobility Goal Achieved 3X per 24 Hours” metric was in the low 30% range. Through a structured, evidence‑based approach that emphasized consistent tracking, clear handoffs, and staff support, April helped improve performance from 31.3% to consistently within 1% of the 60% organizational benchmark for four of the past five months.
April’s impact is driven by her ability to translate quality metrics into meaningful clinical practice. She partnered with Patient Safety Specialists, educated staff on the “why” behind mobility, and fostered strong collaboration across shifts. Beyond mobility, April is a trusted leader and mentor, widely respected for her calm de‑escalation skills, emotional intelligence, and ability to promote safety while preserving dignity. - Austin Erhart – Trauma Surgical Unit / 2026 Magnet Nurse Leader Award. Austin is a transformational nurse leader whose vision, consistency, and data‑driven approach have produced meaningful improvements in patient outcomes, staff engagement, and operational performance on the Trauma Surgical Unit at Medical Center of the Rockies. As Nurse Manager, Austin exemplifies Magnet principles through innovative, evidence‑based practice and a deep commitment to professional development.
One of Austin’s most impactful initiatives was the creation of a dedicated mobility aide role, ensuring mobility is prioritized as a core component of recovery. This innovation improved patient strength, balance, and early mobilization and contributed to a 7.11% reduction in unit length of stay, including a 1.9‑day reduction for geriatric trauma patients. He also led development of a unit‑dedicated discharge flow nurse role, improving throughput, documentation reliability, and allowing bedside nurses to focus on direct patient care.
Austin is equally committed to developing future nurse leaders. He established an early charge nurse orientation program and supports a nurse‑led mentorship initiative that strengthens critical thinking, confidence, and retention. His focus on Structural Empowerment has resulted in a 38% Medical‑Surgical certification rate—well above peer units.
Through active safety leadership, transparent use of data, and strong communication systems, Austin has built a culture of accountability, innovation, and excellence, making him a highly deserving Magnet nurse leader.
Memorial Hospital

Hospital Recognition
MHC: Memorial Hospital Central / MHN: Memorial Hospital North
- American Nurses Credentialing Center (ANCC) Magnet® Designated: 2023.
- U.S. News & World Report Ranked:
- #1 in Colorado Springs four years in a row
- #3 in Colorado
- High performing in over a dozen procedures and conditions, including:
- Stroke and Cardiac Care
- Lung and Colon Cancer Surgery
- Chronic Obstructive Pulmonary Disease (COPD)
- Trauma
- Level I Trauma Center (MHC)
- Level III Trauma Center (MHN)
- Oncology:
- Quality Oncology Practice Initiative (QOPI) Certified through the American Society of Clinical Oncology (ASCO)
- Accreditation Program for Excellence (APEx) Accreditation from the American Society for Radiation Oncology (ASTRO)
- Integrated Network Cancer Program (INCP) Member
- National Accreditation Program for Breast Centers (NAPBC) Accredited
- Breast Imaging Center of Excellence from the American College of Radiology (ACR)
- Lymphedema Center of Excellence (COE) from the Lymphatic Education & Research Network (LE&RN)
- Neuroscience:
- Comprehensive Stroke Center (MHC)
- Primary Stroke Center (MHN)
- Joint commission Disease Specific Certification: Core Spine
- American Board of Registration of Electroencephalographic and Evoked Potential Technologies (ABRET) Accredited Electroencephalogram (EEG) Laboratory
- US News and World Report: High Performing Hospitals – Stroke
- Cardiology
- 2025 Platinum Performance Achievement Award: Chest Pain – MI Registry: NCDR: American College of Cardiology
- Premier Top 50 Cardiovascular Hospitals 2025 – MHC ranked 8th
- American College of Cardiology (ACC) Recognitions:
- Distinction of Excellence: HeartCARE Center
- Chest Pain with Primary PCI and Resuscitation Accreditation
- Electrophysiology Accreditation
- Transcatheter Valve Certification
- Intersocietal Accreditation Commission (IAC) Accreditation:
- Adult Transthoracic Echocardiography
- Vascular Extracranial Cerebrovascular Testing, Peripheral Arterial Testing, Peripheral Venous Testing
- Nuclear/PET: Myocardial Perfusion Imaging
Contributions of Professional Nursing
Colorado Nursing Foundation Nursing Excellence Award Winners 2025
7 Pikes Peak Regional Winners 2025
Exceptional Achievement in Clinical Practice of an Advanced Practice RN
Nicki Seyller DNP, APN, ACCNS-AG, CCRN, SCRN, CRNI
Exceptional Achievement in Clinical Practice of a Community Nursing RN
Andrea Greco BSN, RN, SANE-A, SANE-P
Exceptional Achievement by a Nurse-Led Team
Palliative Medicine & GIP Hospice Team led by John Himberger MSN, FNP-BC, ACHPN
Exceptional Achievement in Nursing Administration by an Executive/CNO
Carolyn Carroll MBAHA, BSN, RN, CCRN-E
Exceptional Achievement in Nursing Administration by a Leader/Manager
Angie Benner BSN, RN, OCN
Exceptional Achievement in Nursing Quality Improvement
Elizabeth Ferriman: BSN, RN, CNRN, CMSRN
Exceptional Achievement in Nursing Education Professional Development
Carri Wright MSN-Ed, RN, NPD-BC, CHSE
3 State Luminary Winners 2025
Exceptional Achievement by a Nurse-Led Team
Palliative Medicine & GIP Hospice Team Led by John Himberger, DNP, RN, FAAN, NEA-BC, FNP-BC, ACHPN
Himberger leads the palliative care team that developed the general inpatient (GIP) hospice program. For patients who are not stable enough to be discharged, this program provides a secure way for them to stay at the hospital. Patients and their families can receive continuous care without significant disruption, and their families can receive bereavement support after the patient dies. The GIP hospice program started in 2023 with two pilot hospice inpatient units. Through its success, the program expanded throughout the hospital in less than a year, and in May 2024, to other UCHealth hospitals.
Exceptional Achievement in Advanced Practice Nursing
Nicole (Nicki) Seyller, DNP, APN, ACCNS-AG, CCRN, SCRN, CRNI
Seyller played a key role in launching a virtual rapid response team, which resulted in more than 250 lives saved between 2022 and 2024. In the past two years, she has developed clinical pathways for patients undergoing alcohol withdrawal, led a quality improvement evidence-based practice change to assist in the identification of ICU patients experiencing delirium, created simulation-based training for critical care charge nurses, and was a major contributor in the implementation of insourcing hemodialysis for inpatients.
Exceptional Achievement in Nursing Education in Nursing Professional Development
Carri Wright, MSN-Ed, NPD-BD, CHSE
Wright developed and facilitated a simulation-based education (SBE) experience for acute care units. Through this experience, she strengthened the clinical reasoning and critical thinking skills of acute care teams. In the past year, she impacted over 130 acute care nurses using the SBE program. Wright also developed a workshop to introduce clinical nurse educators to SBE, which has been adopted across UCHealth.
Parkview Hospital

RN, NEA-BC, FAAN
Pikes Peak Regional Hospital

MSN, RN, CCRN
Hospital Recognition
- Critical Access Hospital.
- CDPHE designated Level IV Trauma Center.
- DNV designated Acute Stroke Ready Facility.
Poudre Valley Hospital

Hospital Recognition
American Nurses Credentialing Center (ANCC) Magnet® designated: 2000, 2004, 2009, 2014, 2018, 2023.

- Primary Stroke Center certification by The Joint Commission and American Heart Association / American Stroke Association.
- American Heart Association / American Stroke Association Get with The Guidelines-Stroke GOLD PLUS Quality Award with Honor Roll Elite 2020 and Target Type 2 Diabetes Honor Roll.
- Nurses Improving Care for Healthsystem Elders (NICHE) member since 2018.
- American College of Surgeons Bariatric Surgery Center Network (ACS BSCN) Accreditation Program – Bariatric Center of Excellence. Re-designated in 2015.
- Patient Centered Medical Home, Level 3 – Family Medicine Center, National Committee for Quality Assurance (NCQA).
- Healthgrades America’s 100 Best Hospitals 2020.
- Watson Health Top 100 Hospitals (Teaching Hospitals) 2021.
- US News & World Report High Performing hospital.
- US News & World Report ranks Poudre Valley Hospital as the #4 hospital in Colorado.
Contributions of Professional Nursing
- Emily Ballantine – Cardiac Unit / 2026 Magnet Nurse Award for Transformational Leadership. Emily is a charge nurse on the Cardiac Unit who exemplifies transformational leadership through her consistent ability to support, empower, and motivate others, particularly on night shift. She leads through reliability, action, and genuine care, creating an environment where staff feel supported, confident, and valued. Emily’s influence is evident without a formal title, as peers regularly look to her for guidance and encouragement.
Education is one of Emily’s greatest strengths. Recognizing the unique challenges of night shift, new graduates, and float staff, she independently developed a cardiac education binder to support overnight clinical decision-making. This resource has improved confidence and care for complex cardiac patients. Emily also provides extensive bedside teaching, especially in ECG interpretation, delivering education in an approachable and non-judgmental manner. Emily contributes to unit-wide improvement by supporting adoption of electronic handoff tools and serving as the night shift Mobility Champion. Through strong communication and leadership, she has fostered safer care, stronger teamwork, and a positive night-shift culture. - Laurie Pyles – Neurology Unit / 2026 Magnet Nurse Award for Structural Empowerment. Laurie is an exemplary nurse on the Neurology Unit whose sustained commitment to professional development, shared governance, and leadership spans more than a decade. As one of the first nurses at PVH to achieve UEXCEL Level 3, and a co-chair during the program’s inaugural year, Laurie has continuously modeled professional excellence and mentored peers in advancing practice standards.
In FY2025, Laurie assumed the role of Unit-Based Council Chair, revitalizing engagement through mentorship initiatives, workflow improvements, and team-building efforts. Her intentional leadership supported succession planning, with multiple UBC members advancing into leadership roles. This year, she expanded her influence as Coordinating Council Chair, facilitating evidence-based discussions and staff listening sessions to elevate frontline voices. Laurie also exemplifies bedside excellence as a core preceptor, maintaining over 90% pain documentation compliance, supporting mobility outcomes exceeding 80%, and contributing to successful ED to Inpatient handoff improvements. She strongly embodies Magnet Structural Empowerment. - Rebekah May – Resource Services / 2026 Magnet Nurse Award for Exemplary Professional Practice. Rebekah exemplifies Magnet’s Exemplary Professional Practice through consistent, high-level interprofessional collaboration that promotes patient safety, dignity, and quality outcomes in complex, emotionally sensitive situations. As a House Supervisor, she extends her impact beyond individual cases to system-level coordination, trauma-informed care, and reinforcement of professional nursing standards
During a neonatal resuscitation, she partnered seamlessly with physicians, nurses, respiratory therapy, and law enforcement to ensure safe, compliant care. After resuscitation ceased, she led a compassionate transition to end-of-life care, enabling skin-to-skin bonding and preserving family dignity. She then advocated for an interdisciplinary debrief to support staff and reduce moral distress.
In another case, she collaborated across disciplines to ensure a pediatric patient’s safe discharge following a family tragedy, addressing unmet needs and advocating for thorough risk assessment.
Rebekah consistently models family-centered care, strengthens communication, and supports staff well-being—ensuring ethical, safe, and accountable practice in all circumstances. - Leah Hochstetler – Neurology Unit / 2026 Magnet Nurse Award for New Knowledge, Innovations, and Improvements. Leah exemplifies the Magnet component of New Knowledge, Innovation, and Improvements through her consistent application of evidence-based practice and innovative approaches to caring for behaviorally complex patients. With nearly 20 years on the Neurology Unit, she recognized the need for proactive strategies to address increasing patient complexity.
She developed an evidence-based Complex Trigger Tool to identify high-risk patients early, enabling proactive discharge planning and shifting care from reactive to preventative. Her work introduced interdisciplinary collaboration, individualized behavior plans, and “Getting to Know Me” tools, resulting in fewer behavioral escalations, reduced restraint use, improved staff safety, and shorter lengths of stay.
Leah also advanced care through technology, securing a WISH Grant to implement Music and Simulated Presence Therapy, promoting comfort and de-escalation.
As a respected Level III RN and mentor, Leah empowers her colleagues through education and modeling, transforming complex care challenges into improved outcomes and stronger team confidence. - Josh Lamarr – ICU / 2026 Magnet Nurse Award for Empirical Outcomes. Josh exemplifies excellence in professional nursing practice through his leadership, innovation, and measurable impact on patient safety, quality outcomes, and workplace sustainability in the ICU. As a charge nurse and Chair of the Skin Committee, he leads interdisciplinary, data-driven initiatives that improve care and strengthen team performance.
He was instrumental in implementing the Leaf Project, a technology-supported turning system to prevent hospital-acquired pressure injuries (HAPIs). Through staff education, collaboration, and compliance monitoring, ICU HAPIs decreased significantly—from 23 in FY24 to just 1 in FY26—reducing patient harm and workload.
His work also led to a substantial decrease in supply costs, improving fiscal stewardship while reducing staff strain. As a leader, Josh advocates for safer practices, mentors colleagues, and promotes accountability and proactive risk identification.
Through innovation, collaboration, and measurable outcomes, Josh consistently demonstrates exemplary nursing practice and a strong commitment to Empirical Outcomes. - Shelby Reimann – Vascular Access / 2026 Magnet Nurse Leader Award. Shelby is an exceptional nurse leader who exemplifies nursing excellence through transformational leadership, structural empowerment, innovation, and measurable outcomes in vascular access care across UCHealth’s North Region. As Vascular Access Nurse Manager, she leads with an inclusive, data-driven approach that prioritizes patient safety, staff engagement, and evidence-based practice while influencing both regional and system-wide improvements.
She successfully transitioned from peer to leader using shared decision-making and strong team engagement, even navigating departmental reductions with creativity and accountability. Through data-driven advocacy, Shelby demonstrated the direct connection between appropriate vascular access staffing, improved patient outcomes, and organizational performance, resulting in increased FTE support. She actively promotes professional growth, supporting certification, career advancement, and contributions to Magnet and Pathway recognition efforts.
Shelby advances Structural Empowerment by fostering a highly skilled, collaborative team that drives system-level initiatives, including vascular access education, documentation improvements, and clinical practice enhancements. Her work has contributed to reduced CLABSI rates at MCR and sustained zero CLABSI events at Greeley Hospital. She remains professionally engaged as a VA-BC certified nurse and subject matter expert in organizational initiatives.
Her leadership in improving central and arterial line practices, developing extravasation prevention pathways, co-creating a central line occlusion pathway, and reinstating the pediatric PICC program has enhanced patient safety, access, and cost efficiency.
Shelby consistently inspires excellence, implements meaningful change, and advances professional nursing practice.
University of Colorado Hospital

DNP, ACNP-BC, FAANP
Hospital Recognition
- #1 US News and World Report in Colorado for 11 years in a row, 2024.
- Quality Oncology Practice Initiative (QOPI) Certification Program 2023.
- American Society of Clinical Oncology 2023.
- Integrated Network Cancer Program (INCP) Commission on Cancer (CoC) 2023.
- American College of Cardiology (ACC) Accreditation Services™ Chest Pain Center with Primary PCI 2022.
- American College of Surgeons (ACS) Level I Trauma Center 2018, 2023.
- Colorado Department of Public Health and Environment (CDPHE) Level I designation 2018.
- American Heart Association (AHA) “Get with the Guidelines” Gold Plus, Target Stroke Elite Honor Roll, and Target Stroke Advanced Therapy Honor Roll 2022.
- American Heart Association (AHA) Comprehensive Stroke Center 2021.
- American Nurses Credentialing Center (ANCC) Magnet® Designated: 2002, 2006, 2010, 2014, 2020, 2025.
- American Nurses Credentialing Center (ANCC) Magnet Prize® Recipient: 2004.
- American Nurses Credentialing Center (ANCC) Magnet Nurse of the Year Award® Recipients: 2011, 2013, 2016, 2023.
- American Burn Association (ABA) Verified Burn Center 2021.
- American Association of Critical Care Nurses (AACN) Beacon Award of Excellence: Neurosurgical Intensive Care Unit 2015
- Baby-Friendly USA, Inc. Baby Friendly® designation 2023.
- Commission on Collegiate Nursing Education (CCNE) accredited Post Baccalaureate Nurse Residency Program 2019.
- National Cancer Institute (NCI) Comprehensive Cancer Center.
The Joint Commission (TJC) Certifications
- Inpatient Diabetes Advanced Certification 2022.
- Advanced Comprehensive Stroke Center Certification 2021.
- Ventricular Assist Device Certification 2022.
- Palliative Care Advanced Certification 2022.
Contributions of Professional Nursing
- Kacey Whittenburg, RN-ICU/2025 UCH Magnet Nurse of the Year Award Transformational Leadership. Kaycey has significantly advanced professional governance and nursing practice through their leadership as Chair of the Clinical Empowerment Council (CEC). Under her leadership, CEC membership grew by 30%, ensuring broader representation across clinical areas. Kacey facilitated bi-directional communication between CEC and unit-based councils, improving efficiency and advancing change initiatives. She expanded a specialized volunteer program for dementia and delirium care, which aimed to improve staff satisfaction and patient outcomes. Not only that but Kacey played a key role in the organization’s compliance with House Bill-22-1401, improving staffing support services. Her efforts have fostered a culture of trust, collaboration, and innovation, significantly enhancing nursing practice and patient care outcomes at UCH.
- Becky Fehlig, Nurse Manager/2025 UCH Magnet Nurse of the Year Award Transformational Leadership. Becky has demonstrated transformational leadership through her innovative initiatives in the creation of the Mobility Technician (MT) program. This program, designed to reduce unassisted falls, led to a dramatic reduction in falls from 7.6 to zero in just six months. The MT program’s success on the ACE unit led to its expansion across all Acute and Critical Care units, improving mobility, reducing falls, and enhancing patient outcomes. Becky’s leadership also resulted in significant improvements in mobility documentation and patient mobility goals, with compliance rising from 54.2% to 72.9% in six months. Her ability to secure resources, foster interdisciplinary collaboration, and drive data-driven improvements has significantly enhanced patient care and staff empowerment at UCHealth.
- Kayla Olson, Charge Nurse Preop/2025 UCH Magnet Nurse of the Year Award Exemplary Professional Practice. Kayla led a transformative initiative to enhance the perioperative pregnancy testing workflow in the Pre-op. She spearheaded a shift from mandatory pregnancy testing to an optional process for patients born female of childbearing age, backed by research from the American Society of Anesthesia. This change empowered patients, respecting their autonomy, and resulted in a reduction of unnecessary tests, leading to improved patient satisfaction and significant cost savings—down from 533 pregnancy tests in January/February to 217 in October/November, saving $199.62 per test. Kayla’s approach fosters inclusivity, patient-centered care, and collaboration across departments while maintaining clinical safety standards. Additionally, she is a key resource on her unit, known for her calm demeanor, expertise in ultrasound-guided IVs, and mentorship of fellow nurses.
- Andrea Elmore, Clinical Quality and Safety Specialist/2025 UCH Magnet Nurse of the Year Award Exemplary Professional Practice. Andrea has dedicated over 20 years to improving patient care and operational efficiency. In 2023, she identified a significant disparity in NTSV C-section rates, particularly among non-English or Spanish-speaking patients, which were at 35.9%. Leading a comprehensive data analysis, Andrea identified key drivers, including communication barriers and inconsistencies in care. She facilitated the formation of a multidisciplinary team to address these disparities, resulting in evidence-based interventions like increasing access to interpreter services and incorporating doula support. Early data shows a reduction in the NTSV C-section rate for non-English or Spanish-speaking patients to 16.5% in late 2024. Through her leadership, Andrea has championed health equity, improved maternal outcomes, and advanced person-centered care, exemplifying transformational leadership by advocating for resources, influencing change, and promoting health equity. Her work directly aligns with the nursing strategic plan, focusing on quality improvement and health promotion.
- Kristi Forsmark, Nursing Supervisor LVAD Program/2025 UCH Magnet Nurse of the Year Award Nurse- Structural Empowerment. Kristi has been instrumental in leading the Mechanical Circulatory Support (MCS) team, particularly in advancing the Left Ventricular Assist Device (LVAD) program. As the Nursing Supervisor of Durable MCS, she oversees the care of LVAD patients, a complex, high-risk group that relies on her leadership for life-saving interventions. Under Kristi’s guidance, the program has become the only LVAD center in Colorado, supporting patients across multiple states. Her initiatives, including the MCS Collaborative Case Review Committee, have significantly reduced LVAD patient readmissions from 3.07% in January 2023 to 0.23% in December 2024, outperforming national averages. Additionally, Kristi’s education efforts have lowered emergency calls from LVAD patients, improving both patient satisfaction and RN work-life balance. Kristi’s leadership fosters interdisciplinary collaboration, enhances patient-centered care, and has brought about measurable improvements in patient outcomes. Her advocacy for best practices and patient safety has made a lasting impact both locally and internationally, earning her widespread recognition in the nursing field.
- Megan Mines Clinical Nurse Specialist-Professional Development 2025 UCH Magnet Nurse of the Year Award Nurse- Structural Empowerment. Megan has led a transformative patient mobility initiative, focusing on improving patient outcomes by enhancing mobility to reduce preventable harm, pressure injuries, falls, and length of hospital stays. Through her expert leadership, she developed and delivered a comprehensive training program for nearly 2000 multidisciplinary clinicians, resulting in a 23% increase in mobility documentation, a 7% improvement in mobility assessment documentation, and a 6% increase in mobility goal achievement. Megan’s exceptional collaboration across disciplines, dedication to education, and commitment to continuous improvement have positively impacted patient care and the professional development of clinicians across the healthcare system.
- Jenna Owen, RN- CARE Clinic/2025 UCH Magnet Nurse of the Year Award Structural Empowerment. Jenna has made a significant impact at UCHealth’s CARE Clinic through her leadership and dedication to oncology care. With 10 years of experience, she has led initiatives that improved staffing, IV skills, and communication, resulting in timely patient care and increased safety. As chair of the Department-Based Council, her mentorship program contributed to a 0% nurse turnover rate, well below the national average of 20.7%. Jenna’s advocacy for infection control and collaboration with EVS has created a safer environment for immunocompromised patients.
- Kelsey Loehr, RN Program Manager/2025 UCH Magnet Nurse of the Year Award Nurse- New knowledge innovations and improvements. Kelsey has made a significant impact in addressing workplace violence and improving staff safety and well-being. Recognizing the increasing incidents of verbal and physical violence in ambulatory care, Kelsey developed and implemented strategies to address these issues. She led the creation of a telephone verbal violence scripting initiative, which empowered staff across nine UCH clinics and other departments to de-escalate challenging situations. Additionally, she initiated a study on cyber incivility, revealing its detrimental impact on nurse morale and turnover, leading to the prioritization of solutions in the UCH Nursing Strategic Plan. Kelsey’s leadership and advocacy resulted in the development of a workplace safety algorithm to address violence and incivility, enhancing staff safety and aligning with UCHealth’s safety goals. Her work has been recognized as best practice by the (AAACN) and has directly improved staff satisfaction, safety, and retention.
- Kristi Van Anderson- Surgical First Assistant OR RN/ 2025 UCH Magnet Nurse of the Year Award New Knowledge Innovations and Improvements. Kristi led a successful project to improve patient safety by addressing the gap in counting breakaway components during spine surgeries. She identified and resolved issues in the existing process by implementing a formal, standardized count of these components between the scrub person and RN circulator and introducing a visual spine count board for tracking. Kristi’s leadership resulted in a decrease in retained breakaway components, and documentation compliance improved steadily, reaching 83% by December 2024. Her work was recognized with a top 10% award for clinical innovation at the 2024 AORN conference, and her manuscript on the process change is moving toward publication. Kristi’s efforts have advanced patient safety, promoted interdisciplinary collaboration, and contributed to evidence-based practice in nursing.
Yampa Valley Medical Center

Hospital Recognition
- CMS 5-star rating in 2021
- ED certified as Level III Trauma Center 2018 (recertified 2019)
- Top 20 Rural & Community Hospitals 2019, 2021
- Top 100 Rural & Community Hospitals 2019, 2020, 2021
- 100 Great Community Hospitals 2018, 2019
Contributions of Professional Nursing
- Michelle Bazile, RN, Med/Surg Resource Nurse and Orthopedic Nurse Navigator; Julie Friese, RN, Med/Surg and ICU; Mary Oamek, RN, Med/Surg and ICU; and Dan Tydeman, RN, OR, moved to Level III in UEXCEL, UCHealth’s Focus on Nursing EXcellence in Clinical Practice, Education and Evidence-Based Practice, and Leadership program, taking an active role in contributing to the improved patient outcomes, education and management (2021).
- Liz Graham, RN, a labor and delivery nurse and lactation specialist at UCHealth Yampa Valley Medical Center in Steamboat Springs, is passionate about her role in supporting women’s health. She was recognized in November 2020 with a Daisy Award for the outstanding care she delivers to patients.
- The Joint Commission recognized a collaborative effort by nurses, physicians, infection prevention, pharmacy, lab and environment services teams on the patient care unit at YVMC for their multi-disciplinary approach and implementation of streamlined processes in the reduction of hospital-onset C. diff. (September 2020)
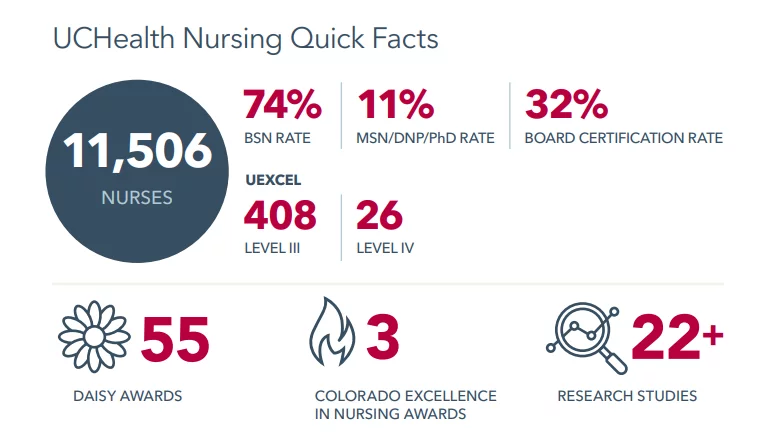
UCHealth Nursing Quick Facts
ANCC Magnet Recognized Facilities

Poudre Valley Hospital
2000, 2004, 2009, 2014, 2018, 2023

University of Colorado Hospital 2002, 2005, 2010, 2014, 2020, 2025

Medical Center of the Rockies
2010, 2016, 2021, 2025

Memorial Hospital Central
2023

Memorial Hospital North
2023
ANCC Pathway to Excellence Recognized Facilities

Greeley Hospital
2024

Longs Peak Hospital
2024
Resources
UCHealth 2025 Nursing Year in Review

UCHealth 2025 Nursing Year in Review
From left, Crystal Rodriguez, graduate nurse with the neuroscience unit at Memorial Hospital Central; Joshua Lamarr, charge nurse III with the intensive care unit at Poudre Valley Hospital; and Lori Wright-Fear, level III nurse with the labor and delivery unit at University of Colorado Hospital share their candid observations and perspectives on nursing through transformational times. Their interview with Chief Nursing Executive Tamera Dunseth Rosenbaum is included among 28 articles honoring nursing excellence and innovations across UCHealth.UCHealth 2024 Nursing Year in Review

UCHealth 2024 Nursing Year in Review
The process for receiving a kidney transplant can be daunting even if English is your first language. Gladiz Martinez, clinical nurse specialist working as a health equity specialist with the UCHealth Transplant Center at UCH, helps Spanish-speaking patients—many of whom have been on dialysis as long as 10 years—receive organ transplants. The successful outcomes of her work are featured among 27 articles honoring nursing excellence and innovations across UCHealth.UCHealth 2023 Nursing Year in Review

UCHealth 2023 Nursing Year in Review
A national increase in incidents of workplace violence against health care workers has not spared Colorado. We’ve intensified focus on verbal violence, which until recently had widely been considered part of the job. Charge nurse Rachel Musenero, collaborated with colleagues to develop a scripting algorithm to support and empower nurses in de-escalating these situations. Her work to support fellow nurses is featured among 29 articles honoring nursing excellence and innovations across UCHealth.UCHealth 2022 Nursing Year in Review

UCHealth 2022 Nursing Year in Review
From left, UCHealth nurses Jill Rozynski, Hope von Gunten, Randi Koch, Jessica Valladares, Adriana Soltero and Gladiz Martinez, represent nursing disciplines across UCHealth in collaboration to improve lives. Their extraordinary work is featured among 26 articles honoring nursing excellence and innovations across UCHealth.UCHealth 2021 Nursing Year in Review

UCHealth 2021 Nursing Year in Review
Assouma Murekeyisoni, a nurse on a floor normally devoted to renal care at UCHealth Memorial Hospital Central in Colorado Springs, joined a nursing colleague to hold the hands of a patient fighting a simultaneous battle against COVID-19 and cancer as she took her last breath. The patient’s daughter later wrote hospital administrators to share her appreciation for the care delivered when she could not be at her mother’s side. This act of compassion through an unprecedented pandemic is featured among 27 articles honoring nursing excellence and innovations across UCHealth.Links
Nursing Professional Development and Recognition Program






