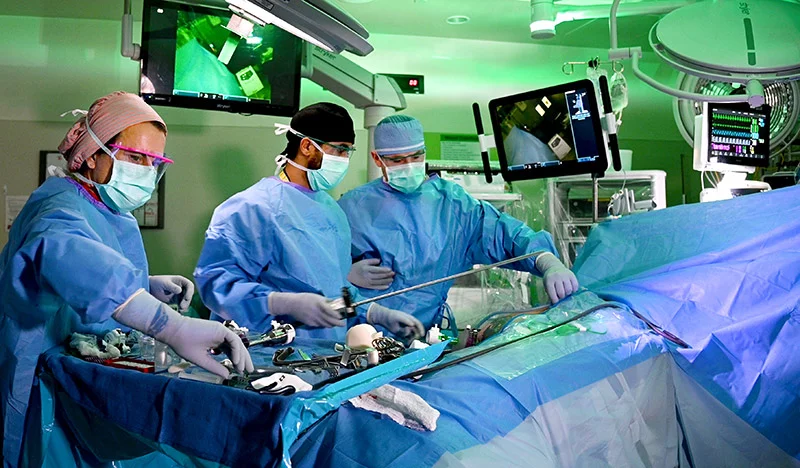
Heart transplants
A heart transplant is sometimes the only option for someone with advanced heart failure who has not responded to medical treatment.



Learn more from our transplant team
Surgical Director Introduction – Heart Transplant
What is involved in a heart transplant evaluation?
What do I need to know about being on a heart transplant wait list?
Heart transplant evaluation
About your heart transplant evaluation
Advanced heart failure means all of your other organs are affected and can begin to perform poorly as well. If medications and adjustments in daily activities and diet aren’t working, your cardiologist may refer you to our heart transplant team for evaluation. You may also refer yourself to our heart transplant team without a primary care or specialist referral.
To be considered for heart transplantation, you will first undergo a comprehensive evaluation and a series of medical tests, including:

- Complete history, physical exam and review of medical records.
- Consultation with a transplant team that includes a transplant cardiologist, transplant nurse coordinator, cardiothoracic surgeon, social worker, financial coordinator, pharmacist, physical therapist and dietitian.
- Blood tests to check for the presence of any infections or exposure to viruses in the past.
- Chest X-ray.
- Echocardiogram to measure how well your left and right ventricles pump blood.
- Electrocardiogram (EKG or ECG) to illustrate the pattern of electrical waves in your heart, which helps the cardiologist examine how your heart is working.
- Pulmonary function tests to measure the function of your lungs.
- Cardiac catheterization, during which a tube is inserted into your neck or groin so the doctor can measure pressure in your heart and lungs.
- Oxygen consumption exercise test to measure your breathing and how much oxygen your body is consuming.
- Kidney function studies, because some medications taken after transplant to prevent rejection can affect the kidneys.
The evaluation process typically takes several days and can be done on an outpatient basis, unless you are already in the hospital, and would then have an inpatient evaluation.
Multidisciplinary approach to determining heart transplant candidacy
A multidisciplinary selection team
After you complete all testing and requirements for your transplant evaluation, your case will be presented to the Heart Selection Committee. This committee is made up of our multidisciplinary team that includes transplant doctors, transplant surgeons, nurse coordinators, social workers, transplant pharmacists, financial coordinators, dieticians and others who are involved in heart transplantation. They will determine if a heart transplant is a safe option for you.
The Transplant Center utilizes a multidisciplinary Selection Committee to determine if you are a candidate for transplant at UCHealth. The criteria used by the Section Committee are fair, objective, and non-discriminatory including but not limited to factors such as race, ethnicity, religion, national origin, age, gender (including gender identity and expression), sexual orientation, or disability. Clinical assessment is a major part of determining your overall health profile and risk with undergoing an organ transplant. A member of the transplant team will share the Committee decision with you.
If you are accepted for a heart transplant, your name and other key medical information are entered into the United Network for Organ Sharing (UNOS) database and put on the waiting list for a donor heart. This national, computerized listing is maintained to ensure fair and equitable distribution of donated organs.
Candidate prioritization
We follow the UNOS system for prioritizing transplant candidates. For this system to work, it relies on organ procurement organizations, called OPOs. OPOs match and distribute donated organs, 24 hours a day, 365 days a year. The OPO in our region is Donor Alliance (DA). DA is responsible for the coordination, retrieval and distribution of organs in Colorado and Wyoming.
Heart transplant waiting period
Once we have placed you on the UNOS list, you may wait for weeks, months or years for a donor heart depending on your degree of illness and other factors. We strongly recommend that you have a supportive network of family and friends to help you during this stressful time.
Getting ready for a heart transplant
Supporting heart health while you wait
We may recommend that you participate in cardiac rehabilitation to help improve your health before and after your heart transplant. If medical therapy fails to support your vital organs as you wait for a donor heart, we may recommend you have a device implanted to support your heart while you wait for a donor organ, such as a left ventricular assist device (LVAD). These devices are also referred to as a bridge-to-transplant because they stabilize your condition until a donor heart is available.
Be ready when the call comes
A donor heart needs to be transplanted within four hours after being removed from the donor. We expect you to arrive immediately after being notified of a potential donation, so be prepared with a suitcase packed with everything you’ll need for your hospital stay, including an extra 24-hour supply of your medications.
Heart transplant surgery
Heart transplant surgery is open-heart surgery. It usually follows these steps:
- You will receive general anesthesia before and during the procedure, which will take several hours.
- Your cardiac surgeon will make an incision in your chest, and will separate your breastbone and open your rib cage.
- A heart-lung bypass machine will keep oxygen-rich blood flowing throughout your body.
- Your cardiac surgeon removes your diseased heart, then sews the donor heart into place.
- Next, he/she attaches your major blood vessels to the donor heart. The new heart usually starts beating when blood flow is restored, but sometimes we use an electric shock to make the donor heart beat properly.
- A ventilator will help you breathe until you are awake and able to breathe on your own.
- You will have tubes in your chest to drain fluids from around your lungs and heart.

After surgery, you’ll receive fluids and medications through intravenous (IV) tubes, including pain medication to help you recover.
Post-surgical care after a heart transplant
Expert care after your surgery
After the transplant, you will receive follow-up care by your heart transplant team. Your cardiologist and care team will regularly review your lab work, cardiac biopsies and echocardiograms.
You will need to stay within the metro Denver area for a minimum of three months after your transplant if you live more than three hours from our hospital. The transplant team, in conjunction with your primary care physician, will handle the long-term follow-up. Having a heart transplant is a lifelong commitment. You must understand and participate fully in taking care of yourself with exercise, a healthy diet, taking your prescribed medications and ensuring that you make it to your medical appointments after your transplant.
After surgery, we will put you on medications for life to prevent rejection and infection. It is not unusual to experience some rejection following a transplant. The transplant team follows your recovery closely and is prepared to successfully treat any signs and symptoms of rejection.
A major side effect of immunosuppressant medication is the increased risk of infection due to a reduction in your natural immunity. Your transplant care team will give you separate medications to prevent infection and will work with you to keep them both in balance. We will monitor your cardiac function and response to all medications.
Complications and risks following heart transplant surgery
Complications
Heart transplant surgery is open-heart surgery, a serious procedure that carries the possibility of certain complications, including:
- Bleeding
- Blood clots
- Infection
- Heart attack
- Stroke
- Death
Problems with coronary arteries
After your transplant, the walls of the coronary arteries in your heart could thicken and harden. This could lead to cardiac allograft vasculopathy (CAV), making blood circulation difficult and possibly leading to a heart attack, heart failure, abnormal heart rhythms (arrhythmias) or sudden cardiac death. We may recommend annual tests to monitor for CAV.
Biopsies
To determine whether your body is accepting or rejecting your new heart, we will perform frequent heart biopsies to test your heart tissue during the first year after your transplant. After the first year, we will significantly reduce the number of biopsies you need.
Risks
- Rejection
- Mental confusion
- Seizures
Rejection: what it means
Your immune system might attack a donor heart as if it is a foreign object that’s not supposed to be in your body. You will receive immunosuppressant medications that reduce the activity of the immune system, but around 10% of heart transplant recipients still have some signs of rejection that need additional treatment during the first year after transplantation. Usually an adjustment of medications is enough, but if you miss doses, the rejection can be very serious so it’s critical that you follow your doctor’s instructions.
These anti-rejection drugs suppress your immune system, which makes you more susceptible to infections, particularly in your lungs. To help, you should:
- Regularly wash your hands and brush your teeth and gums.
- Protect your skin from scratches and sores.
- Avoid sick people and crowds.
- Get all appropriate vaccinations.
Medication side effects
The immunosuppressants you’ll take for the rest of your life may cause kidney damage and other problems, like high blood pressure, high cholesterol, diabetes and osteoporosis. Immunosuppressants decrease your ability to fight infection, so during your first year post-transplant, you may develop an infection that requires hospital admission. The risk of infection decreases over time as we decrease the amount of your immunosuppressants.
Increased cancer risk
Immunosuppressants can put you at a greater risk of skin cancer, non-Hodgkin’s lymphoma and other solid tumors. We will perform regular checkups to detect the development of cancer.
References
American Heart Association (AHA). Heart Transplant – https://www.heart.org/en/health-topics/congenital-heart-defects/care-and-treatment-for-congenital-heart-defects/heart-transplant
MedlinePlus: National Library of Medicine. Heart transplant – https://medlineplus.gov/ency/article/003003.htm