
Just a few years ago, Elaine Restauri’s entire life revolved around pain.
She tried to avoid it through medications prescribed to calm the “thunder” inside her head.
She tried to manage it by forsaking activities she had once loved, like horseback riding and gardening, because any motion would make her nauseous and dizzy.
She tried to mitigate it by squeezing a day’s worth of work and errands into a few morning hours, treading lightly around her home in special padded shoes to cushion physical movement.
And she tried to keep her spirits up, despite spending much of the day in bed, as lying prone gave her a slight respite from the constant torment she experienced.
“It was blinding. It was horrible,” said the 69-year-old Elaine. “The pain was so great that you can’t process things rationally in your brain. Somehow, I learned to live with it.”
Permanent relief finally came from Dr. Andrew Callen, a UCHealth neuroradiologist and pioneer in diagnosing and treating patients with spontaneous cerebrospinal fluid (CSF) leaks.
Cerebrospinal fluid (CSF) protects the brain and spinal cord from injury
CSF is a clear fluid surrounding the brain and spinal cord and has several roles, including protecting the brain and spinal cord from injury and providing nutrients. It’s contained by a thick connective tissue called the dura, the outermost layer of membrane called meninges that cushions the central nervous system.

People can incur CSF leaks through medical procedures such as spinal taps and epidurals, as well as through serious accidents or injury. However, spontaneous leaks — when the fluid drains through a tiny tear or hole in the dura surrounding the brain and spinal cord without any identifiable cause — have proven challenging for both patients and the medical community.
These spontaneous leaks can be tiny and sometimes numerous in the skull or spine. It is a rare malady, occurring in about five of every 100,000 people per year, and more women than men suffer from it.
“We were a match made in heaven,” Elaine said of Callen, who is the director of the University of Colorado CSF Leak Program. “He knew immediately what I needed and turned my life around.”
Callen has made it his mission to help patients such as Elaine, who have spent years in a frustrating medical merry-go-round, as they often have been seen by numerous physicians and specialists, neurology clinics and emergency rooms. The nuances of CSF are complicated, and even when patients receive a positive diagnosis, they may experience setbacks and need follow-up procedures before a successful outcome.
He is excited about a new CSF clinic opening this month at CU-Anschutz with a designated space to help treat patients with spontaneous CSF leaks. He will lead the clinic, along with a team of radiologists, neurologists, and neurosurgeons, to provide cutting-edge testing and treatment for this condition.
Venous fistula leaks: a syndrome just discovered in 2014
Callen is a national expert in treating spontaneous CSF leaks, and specifically, venous fistula leaks, in which the fluid leaks directly into a vein, making them incredibly difficult to detect through most imaging techniques. Physicians did not even discover these leaks until 2014.

He explained that the balance of fluid and blood in the brain and spine is a delicate one – CSF patients experience an aberration that occurs when that precise communication goes awry.
“We tend to see patients with a long and complicated history,” he said. “Part of the problem is that each patient might have their own set of unique symptoms. Many of them have been written off by certain clinicians as having a CSF leak because their symptoms don’t fit neatly into a box.”
For people suffering from migraines and other headache issues who wonder if they might have a CSF leak, there is nearly always one telltale sign: Almost all CSF patients have “orthostatic” symptoms, meaning they are worse when they are standing and better when they lie down. In addition to headaches, people might also experience a sense of pressure, ringing in their ears, changes in vision or hearing, dizziness, forgetfulness or personality changes.
“It can be much more than a headache for many of these patients.” Callen said. “It can be a terrible, painful and horrible ordeal. It can cause vision problems, confusion, and a whole constellation of psychological and neurological issues if it goes undiagnosed.”
Would Elaine ever get better?
This had been true for Elaine.
A mother of three who lost her husband when her youngest daughter was only six months old, she raised her family in the Pittsburgh area, making a life for herself as a graphic artist. In 2009, Elaine relocated to Colorado to be with her three daughters. She is an independent and happy woman who loved gardening and painting with watercolors and acrylics.
Her problems began in 2012. After returning to Denver from an international flight, her head began to hurt in a way she could never have ever imagined. She initially assumed she was dehydrated, jet lagged or had a sinus infection. After six weeks of horrific head pain, she sought medical help and was given an initial diagnosis of meningitis before physicians suspected a CSF leak and used a procedure using her own blood to patch it. This worked temporarily, but she had to seek treatment again in 2019.
By the summer of 2021, her symptoms were so awful that she spent much of her days in bed. She experienced nausea, vomiting and vertigo in addition to head pain.
Her daughter, Dr. Nicole Restauri, a UCHealth thoracic radiologist and a colleague of Callen, was determined to get her help. She had watched her mother physically and mentally decline from a vibrant and independent woman who had raised three daughters alone to a shadow of her former self.
“She had been suffering for years,” said Nicole. “Until recently, no one knew there was a definitive way to treat it.”
After Elaine met with Callen, he performed an MRI of her brain and entire spine. The findings of those studies suggested that she was suffering from a CSF-venous fistula, where her CSF was abnormally leaking into a vein. It’s not always known why these leaks occur – a leading hypothesis for creating CSF-venous fistulas is damage to a structure called an arachnoid granulation. In other non-fistula leaks, perhaps some sort of “microtrauma” occurs, causing a hole in the dura.
 “When leaking slowly, they can be particularly hard to detect,’’ he said.
“When leaking slowly, they can be particularly hard to detect,’’ he said.
“The understanding of these spontaneous leaks has exploded over the past two decades, and our work with venous fistula leaks is even more new,” he said.
Despite Nicole working in the radiology field, even she is amazed at the technology that detected her mother’s CSF leaks – something she wants more people to know about so they, too, can get help.
“To be honest, I didn’t even know how specific and precise the treatment could be,” she said. This type of procedure illustrates the power of how advanced imaging can be used to treat patients, she said.
For Elaine, the continual loss of CSF fluid had caused her brain to actually sag into the cradle of her skull since it lacked the proper amount of fluid to help it float properly.
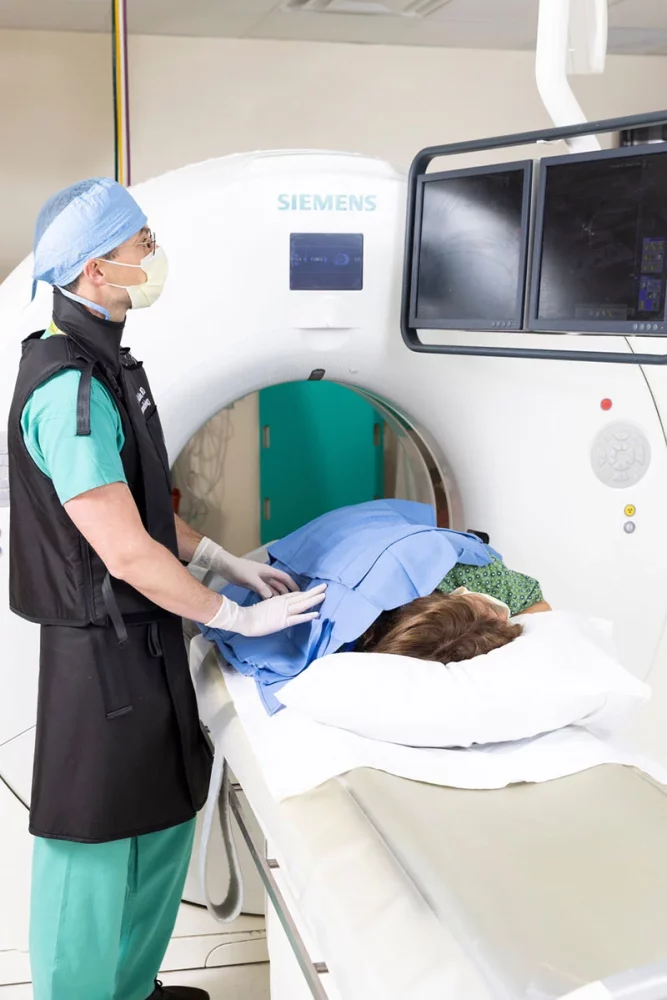
Callen was able to successfully treat Elaine through specialized testing called dynamic myelography to diagnose her condition. Through myelography, a dye is used in imaging to look for problems in the spinal canal while radiologists maneuver the patient into various positions on the exam table to try and find the leak. When one is found, he can patch it with a patient’s own blood drawn through an IV, then injected into the leak, or with a substance called fibrin glue (which includes strong clotting components of blood), that creates a super clotting mixture, he said.
In more extreme cases, when neither a blood patch nor fibrin glue will work, he will refer a patient for surgery where they will have the vein clipped or embolized to stop the leak.
Trained at University of California San Francisco School of Medicine, one of the initial hospitals to do spontaneous CSF research, he saw firsthand how a proper diagnosis could be life-changing. He recalls one of the first patients he treated who was finally properly diagnosed with spontaneous CSF had been misdiagnosed for years – with ALS, also known as Lou Gehrig’s Disease.
“These patients were told it’s all in their head when really, it’s all in their spine,” he said.
After years of pain, finally, relief from CSF leaks and a return to normal
Attaining her equilibrium in body and spirit after what seemed like an eternity of imbalance can be challenging for patients, and Elaine is no exception. It’s common for them to produce too much CSF after their leak is sealed, which she also experienced, although the fluid production quickly corrected itself after a few weeks.
In addition, the years that Elaine lived with CSF caused some permanent damage to parts of her body: Her voice can be raspy because of nerve damage to her vocal cords, and she suffers from a pinched nerve in her spinal cord that affects her right shoulder and arm. From the many years of experiencing vertigo, she is sometimes off balance and can veer toward the left, into a wall, if she’s not careful. But these are small ailments compared to what she had been dealing with.
“I’m otherwise in great shape,” she said. “When you have a CSF leak, it’s amazing how you adapt. But now, I can move and do what I want to do,” Elaine said. “When this happens to your head and body your senses become so heightened to pain, even eating a particular food with a certain chemical in it will trigger pain in your head.”
Trying to make up for lost time, she’s been busy traveling, gardening, working on her art and even thinking about getting back on a horse.
“I feel so much better. I feel normal,” she said, adding that she has been headache free for a year and a half.
For Callen, seeing patients transform into the person they once were motivates him and his colleagues.
“It’s been very rewarding and incredibly satisfying to help these patients – it’s a big part of the excitement around this research and clinic,” he said.
For Elaine’s daughter, seeing her mom blossom and bloom again, like the flowers in her beloved garden, is priceless.
“It saved her. It gave her back her life.”
