
Veronica Wilkins suddenly began feeling intense chest pains that seemed to shoot right out her back. She was 36 weeks pregnant and was being monitored for preeclampsia after being diagnosed with gestational hypertension, but she knew it wasn’t normal pregnancy pain. It was crippling, so she called 911.
“I remember telling [my teenagers] to get the young kids out of the house,” Wilkins recalled. “I really thought I might die right there.”
The 39-year-old, soon-to-be mother of six was experiencing a dissecting aneurysm in her aorta.
The aorta is the largest artery in the body, running down the front of the backbone. It supplies blood to the circulatory system. In some cases, the wall of the aorta weakens and bulges in what’s called an aortic aneurysm. However, instead of bulging, Wilkins’ thinned aortic walls tore between its layers — a dissecting aneurysm. This causes blood to flow inside the separate layers, diminishing flow in the artery.
UCHealth cardiovascular surgeon Dr. Mark Guadagnoli was at Medical Center of the Rockies in Loveland when the call came in.
“This is a case with 200 percent mortality because we can lose mom and baby,” Guadagnoli said. “I have experience with this type of case [a pregnant women needing emergency cardiovascular surgery], so fortunately I knew how to manage the problem.”
Guadagnoli had UCHealth LifeLine transport Wilkins from Longmont United Hospital to MCR.
“This was a high-risk call, so we grabbed our fetal monitor to take with us,” Air Link’s Wyandt Holmes said.

UCHealth’s northern Colorado critical care transport team, which includes both ground and air services, underwent special training in early 2016 to transport expecting mothers. The training included how to monitor the mother and baby with a new high-tech fetal monitor.
But when the crew received Wilkins, they weren’t able to use the new equipment because they had to position Wilkins to address her heart emergency, preventing the fetal monitor from functioning properly. But Holmes’ training prepared him for that as well.
“We found out that the baby’s only risk was the mom dying,” he said. “You have to decide who you are treating — a baby that’s fine or a mom that will die. If we didn’t address the aneurysm, the other parts would be irrelevant.”
Meanwhile, Guadagnoli gathered his team for emergency open-heart surgery and simultaneously called labor and delivery so they could prepare a team for an emergency C-section in an operating room reserved for cardiovascular surgeries.
“When I was wheeled on the gurney from the helipad, there were just a couple people, and from that point things got so real for me and they were all moving so fast that I sort of shut down,” Wilkins said. “There were so many people in the OR, and they were all racing around me, that I focused on just me and I prayed.”
Only July 18, 2016, only minutes after Wilkins arrived in the operating room at MCR, the healthy, 6-pound, 13-ounce Thane Ashley Corlett-Wilkins was delivered via C-section. Wilkins’ open-heart surgery to fix her aneurysm and replace her aortic valve started immediately after the delivery nurses cleared the room.

“Our focus was the baby,” said registered nurse Carrie Guffey. “Once the baby was out, we backed down and let the other teams take over. Mom was in surgery, but we had the dad, so we grabbed him to bond with the baby.”
MCR, as with all UCHealth hospitals, is Baby-Friendly, a certification identifying hospitals that support such things as breastfeeding and skin-to-skin bonding.
“Thane did miraculously,” Guffey said. “We were prepared for anything but pleasantly surprised. As the newest member of their family, we needed to make sure he was able to bond. We think of our patients as being the whole family. And when we put that baby in the dad’s arms, despite everything going on with mom, you could see them both relax a bit.”
Wilkins remained in surgery, during which time the dissection was surgically corrected and an artificial valve replaced her damaged aortic valve.
The aortic valve opens each time the heart pumps to let out a burst of oxygenated blood, and then it closes. It’s important that it works properly. UCHealth Heart and Vascular Center – Medical Center of the Rockies performed 240 valve replacements in patients between July 2015 and June 2016, along with attending to over 30 emergent aortic dissections and aneurysms. Guadagnoli said Wilkins’ surgery was very high risk.
“It’s unusual to have this combination, but the multidisciplinary coordination that happened went perfectly,” he said. “We could have lost mom and baby, but we saved both.”
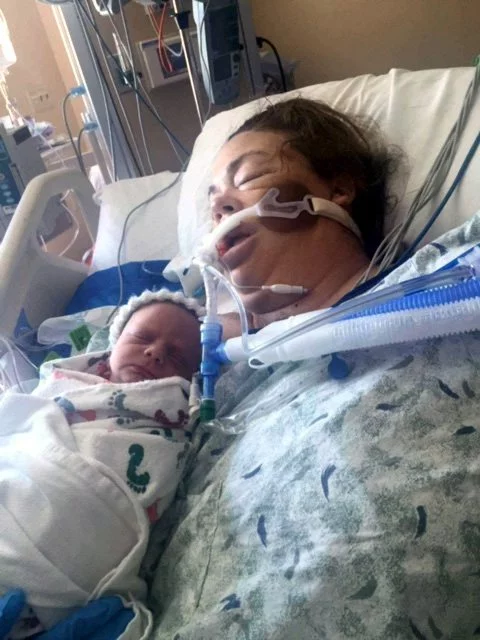
Wilkins woke to find her baby and husband by her side in the cardiovascular intensive care unit.
“They let dad and the baby stay with me in the ICU, and that meant a lot to me,” she said. “The nurses were so good to me. They would come into the ICU, put him in my arms and then wait hours while I held him. I also think I saw almost every cardiac surgeon at MCR, and they made sure I wasn’t going to go home until I was ready.”

Wilkins spent a week in the ICU and another in an inpatient room. A strong woman, used to doing things for herself, she struggled with her post-surgery self, but her nurses were very supportive.
“I told them I needed lots of encouragement,” Wilkins said. “I didn’t know how I was supposed to feel. I didn’t know how I was supposed to be doing. I didn’t feel like I was making any progress. It was hard.”
But she did make progress, and each day she became a little stronger. During an interview with UCHealth Today 10 weeks later, Wilkins said she had finally gotten a bit of her old life back.
“Yesterday was a big deal for me,” she emailed to UCHealth staff, along with a photograph, on Sept. 29, 2016. “I drove a big ol’ Belgian draft (horse) yesterday, and it was my first time ever driving. I am looking at keeping involved and spending time with my horses, and this could be how I do it. I would love it if Dr. Guadagnoli could see that I am trying to get back to as normal life as possible. He did an amazing thing for me … He gave me a chance to make it, and I have.”
