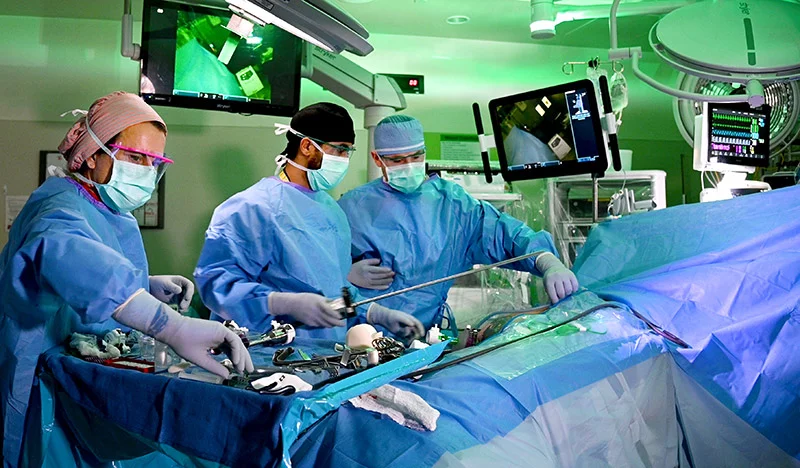
Liver transplants
For over five decades, we’ve given hope to patients with liver disease.
Liver failure can happen over time—or quickly. Liver transplant is your only option if you have liver failure that can’t be controlled with other treatments, or if you have a primary liver cancer.
Chronic liver failure or cirrhosis can occur as a result of any chronic liver disease. The most common causes of cirrhosis include alcoholic liver disease, non-alcoholic fatty liver disease, viral hepatitis such as hepatitis B and C, autoimmune diseases and genetic conditions.
Acute liver failure (fulminant hepatic failure) occurs quickly—over a few days to a few weeks—and can be due to a viruses, toxins or be medication-induced. Sometimes the cause is unknown.
Learn more from our transplant team
Dr. Burton, Liver Transplant Medical Director
Dr. Pomposelli, Liver Transplant Surgical Director
Amy Huntsman, Transplant Nurse Coordinator
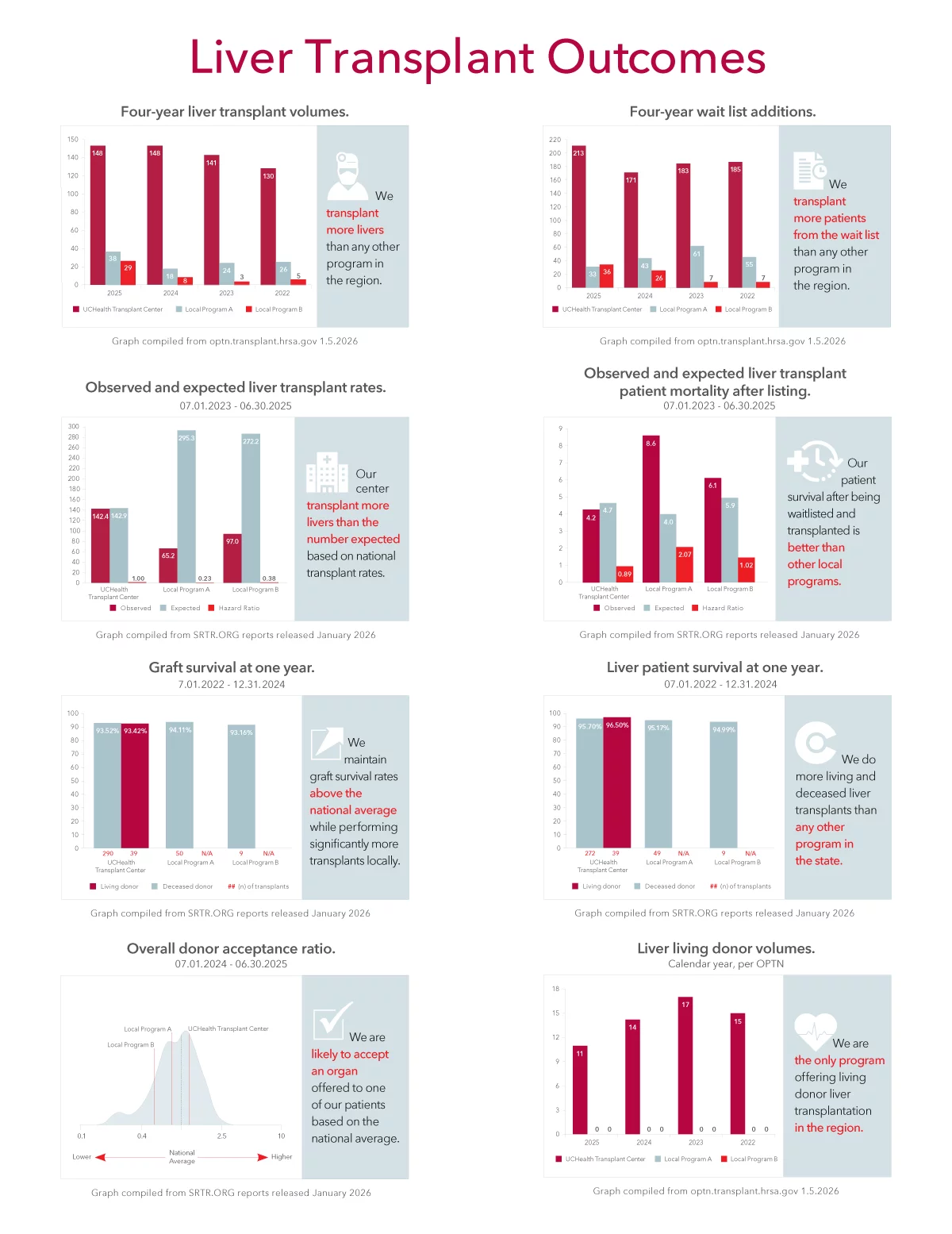
UCHealth Liver Transplant Outcomes
Compare UCHealth program data to others in the region.
We’re pioneers in liver transplant
The first successful liver transplant in the world was performed at our hospital in 1967, and since pioneering this surgery, we’ve performed thousands of liver transplants in adults and children from all over the country. We also have extensive experience in performing living donor liver transplants. In 1997, we performed the first living donor liver transplant in an adult.
We have been recognized as a top-performing academic medical center by University Health Consortium. If you are experiencing acute or chronic liver failure, your hepatologist may refer you to us to see if you are a good candidate for a liver transplant.
Liver transplant evaluation
We reserve transplantation for patients whose liver disease is irreversible and cannot be adequately treated any other way. To be considered for a transplant, you will meet with a transplant hepatologist for an evaluation and testing, which will include:
- Complete history, physical exam and review of medical records.
- Blood tests to evaluate the severity of liver dysfunction.
- CT scan or MRI to evaluate the size of your liver, presence or absence of liver mass, and the status of bile ducts and blood vessels.
- EKG and echocardiogram to assess heart function.
- Chest X-ray and pulmonary function tests to evaluate lung function.
- Additional testing may be needed based on results of prior exams.

You will also meet with a transplant surgeon, a transplant nurse coordinator, a transplant social worker, a financial coordinator and a dietitian.
Our standard evaluation process is tailored to your needs and typically takes two days. It is done as an outpatient, or as an inpatient for those who are in the hospital and are too sick for an outpatient evaluation. We encourage you to bring a close family member or friend with you for support and to ensure that all of your questions and concerns are addressed.
Multidisciplinary approach to determining liver transplant candidacy
A multidisciplinary selection team
After you complete all testing and requirements for your transplant evaluation, your case will be presented to the Liver Selection Committee. This committee is made up of our multidisciplinary team that includes transplant doctors, transplant surgeons, nurse coordinators, social workers, transplant pharmacists, financial coordinators, dietitians and others who are involved in liver transplantation. This committee meets every week and determines if a liver transplant surgery is safe for you. They will also discuss a plan of care for you after transplant.
The Transplant Center utilizes a multidisciplinary Selection Committee to determine if you are a candidate for transplant at UCHealth. The criteria used by the Section Committee are fair, objective, and non-discriminatory including but not limited to factors such as race, ethnicity, religion, national origin, age, gender (including gender identity and expression), sexual orientation, or disability. Clinical assessment is a major part of determining your overall health profile and risk with undergoing an organ transplant.
Your waiting list placement
Your hepatologist or transplant nurse coordinator will inform you of the committee’s decision and plan. If you are accepted for a liver transplant, your name and other key medical information are entered into the United Network for Organ Sharing (UNOS) database and put on the waiting list for a donor liver. This national, computerized listing is maintained to ensure fair and equitable distribution of donated organs.
Part of your placement on the UNOS list includes your Model for End-Stage Liver Disease (MELD) score (or PELD score for children younger than 12). MELD scores estimate the risk of death within 90 days without a transplant. MELD scores range from 6 to 40—the higher your MELD score, the more dire your situation.
Getting ready for a liver transplant
While you are waiting for a transplant, stay as healthy and as active as you can. This will make you better prepared for the transplant, and may also help your recovery. Keep these recommendations in mind:
- Take all medications as prescribed.
- Follow your diet and exercise guidelines.
- Don’t smoke.
- Keep all appointments with your health care team.
- Participate in healthy activities, including spending time with family and friends.
Liver transplant surgery
Once your transplant team is ready to proceed with your surgery, you’ll be given general anesthesia for the procedure. During the procedure, your transplant surgeon makes an incision across your abdomen to access your liver.
Deceased donor liver transplant
Your transplant surgeon replaces your old liver with the donor organ and attaches it to the major blood vessels and bile ducts. Surgery can last up to 12 hours. You will be taken directly to the ICU if indicated, but many of our patients will go to the recovery room before going to our specialized transplant unit.
Living donor liver transplant
If you’re receiving a liver transplant from a living donor, your surgeon transplants a portion of the donor’s liver into your body. We first operate on the donor, removing the portion of the liver for transplant. Then we remove your old liver and place the donated liver into your body, connecting your blood vessels and bile ducts to the new liver.
Both the transplanted liver in your body and the remaining liver in the donor’s body regenerate rapidly, reaching normal volume within a couple of months.
You will stay in the hospital post-transplant from five to 12 days, depending on your recovery. You may return to work as early as six weeks after surgery, depending on your condition.
Complications and risks
Complications and risks following liver transplant surgery include but are not limited to:
Complications
- Bleeding
- Liver non-function
- Infection
- Delayed return of bowel function
- Pain
- Organ failure
- Death
Risks
- Rejection.
- Bile duct complications, including bile duct leaks or shrinking of the bile ducts.
- Blood clots.
- Mental confusion.
- Seizures.
- Recurrence of liver disease in the transplanted liver.
Rejection
Even with the best possible match between you and the donor, your immune system will treat your new liver as a foreign body and will try to attack and reject it. This risk is highest immediately after transplant, and will reduce over time. We will put you on immunosuppressant medications to suppress your immune system, which may have side effects, and you will take them for life. These anti-rejection drugs suppress your immune system, which makes you more susceptible to infections.
Post-surgical care after a liver transplant
Specialized care after your surgery
After surgery, you will recover in a specialized unit for transplant patients. Your team will perform blood tests to check the function of your new liver and level of medications, and they will monitor you for any signs of rejection and infection. They will also give you and your family instructions about nutrition and how to administer your medications, as well as how to gradually increase your activity level.
After your discharge from the hospital, you will need to stay within the metro Denver area for several weeks, as you will receive follow-up care in our transplant clinic twice a week for the first few weeks, and as directed by your nurse coordinator after that. The transplant team will direct long-term follow-up with your primary care provider.
You’ll need to take anti-rejection medications for the rest of your life to help prevent your body from rejecting the donated liver. These medications work by suppressing your immune system, so they can increase your risk of infection. Your doctor may prescribe additional medications to help with this.

References
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). Definition & Facts of Liver Transplant (https://www.niddk.nih.gov/health-information/liver-disease/liver-transplant/definition-facts)
American Liver Foundation. Liver Transplant (https://liverfoundation.org/liver-diseases/treatment/liver-transplant/)
United Network for Organ Sharing. Liver Transplant Living (https://transplantliving.org/organ-facts/liver/)