
Erin McDaniel’s first and second pregnancies started out the same way.
“They were easy, with lots of energy,” she said.
“Sometimes too much energy,” her husband, Graham, countered.
The pregnancies finished completely different.
“Eddy was born at almost 41 weeks via C-section. Besides being breech, there weren’t any problems – she was a healthy little girl,” recalls Erin. “With Mimi, she felt to be in the same breech position as Eddy was. She, however, entered the world at 35 weeks via emergency C-section and spent almost a month in the special care nursery.”
When it gets real, real fast
As a freelance videographer, Erin’s days are flexible but full, with client meetings, shoots and editing sessions scattered on her calendar.
“The weekend before my water broke with Mimi, we filmed a wedding and the day before, I was on a real estate video shoot,” she said. “We were still working on remodeling projects and the baby’s room. Eddy and I were making cupcakes when my water broke – she thought my water bottle broke.”
Erin called UCHealth Women’s Clinic in Steamboat Springs at 4:15 p.m. on Sept. 11 and was told to come in. Following an amniotic fluid test to determine that her water had indeed broken and the amniotic sac that surrounded the baby had broken, “it got real, real fast.”
“We didn’t pack a bag and had a toddler in tow,” said Graham. “We didn’t think at that point we were staying for a month.”

Dr. Diane Petersen saw Erin and determined that delivery was imminent.
“I was concerned about the date being 9/11 and asked if we could wait until the next day, but Dr. Petersen said water breaks for a reason and the baby wanted to come now.”
“With preterm premature rupture of membranes (PPROM), large studies have shown that delivery is safer for baby and mother. There is a 15-25% chance of infection with PPROM and also a 2-5% risk of placental abruption, meaning the placenta tears away from the uterine wall,” said Petersen. “Add in Erin’s history of a previous cesarean section due to breech presentation and the fact that she was having mild uterine contractions, it was clearly time for the baby to be delivered. While delivery at 35 weeks was unexpected, she had grown a healthy baby to 35 weeks, which put the baby at an advantage.”
“I was still naïve that she was going to be born at 35 weeks,” said Erin. “There wasn’t the same pomp and circumstance surrounding everything that we felt when Eddy was born.”
“We didn’t do research on what it was like to have a preemie, as we never thought she’d come this early,” said Graham.
Distress at 35 weeks

Once Erin and Graham were in the operating room and the drape went up at Erin’s chest, the difference in experience between her first delivery and this one were stark.
“It was one of the scariest moments of my life,” said Graham “It had been a few minutes and I could tell from my vantage point something wasn’t going right as Dr. Petersen worked quickly to deliver our daughter.”
She was born at 7:51 p.m., was 17.75 inches long and weighed 4 pounds, 9 ounces. She was five weeks early.
“They didn’t show me the baby right away when she delivered, and that was my first window into this was different than with Eddy,” said Erin. “I knew the doctors had her and kept asking Graham why he wasn’t going to see the baby.”
“She was grey. That is a tough visual to get out of your head. And not hearing her cry right away…,” said Graham. “You could tell she was struggling. The first hour of her life she was put through the ringer, but we had such trust in the doctors and nurses who were taking care of her.”

Along with a team of nurses, pediatrician Dana Fitzgerald and Allyson Daugherty, a neonatal nurse practitioner with Children’s Hospital Colorado who cares for newborns in the special care nursery in Steamboat Springs at UCHealth Birth Center, worked feverishly to stabilize the baby.
“Respiratory Distress Syndrome is very common in babies who are born prematurely and was one of my main concerns,” said Daugherty. “This condition is due to a deficiency in a protein called surfactant, which is produced by the cells in the lungs to help reduce surface tension. Surfactant is naturally produced starting at 28-30 weeks’ gestation, but not in abundance until the last several weeks of gestation.”
When mothers know they are going to deliver prematurely, a steroid shot called betamethasone can be given to help boost the fetus’s surfactant production. But the baby’s arrival was unexpected so there wasn’t time for Erin to receive the steroid shot.
“After the baby was born, we were able to give her surfactant through a breathing tube that went directly into her lungs to help reduce the surface tension to keep her lungs open, allowing her to breath easier,” said Daugherty. “After the medication was given, we were immediately able to remove the breathing tube and then use noninvasive modes of respiratory support.”
While the baby’s respiratory distress began to improve, Graham’s distress continued.
Feeling helpless
“It felt like an episode of ER. They’re going to town on a little four-pound baby and there wasn’t a thing I could do,” he said. “I kept thinking how I didn’t want to go home without my wife or my new daughter. I didn’t want to be a single dad. But I knew Erin would be ok because the C-section went well. But this wasn’t how it was all supposed to happen.
“It reminded me of how my grandparents went out of life, how they looked when I said goodbye to them – and this was how my daughter was starting her life,” continued Graham. “You’re literally helpless and there’s nothing you can do about it.”
Because the baby was born so early, had the surfactant not worked, the possibility of needing to transfer to a larger facility existed.
“That would have been on a whole other level of what ifs,” said Erin.
“I try to make sure parents understand, as best they are able, what types of infants we can keep here, and which ones we can’t, so they aren’t blindsided if their child needs flown to Denver,” said Fitzgerald. “I was fairly confident she wouldn’t need to fly, but wasn’t 100%. This is a perfect case of why it’s so great we have a partnership with Children’s Hospital Colorado and their neonatal nurse practitioners, because without them and our Level II special care nursery in Steamboat Springs, this little one would been flown to Denver and hospitalized there for weeks, instead of remaining locally at YVMC.”
Two hours after she was born, Erin finally met her daughter.
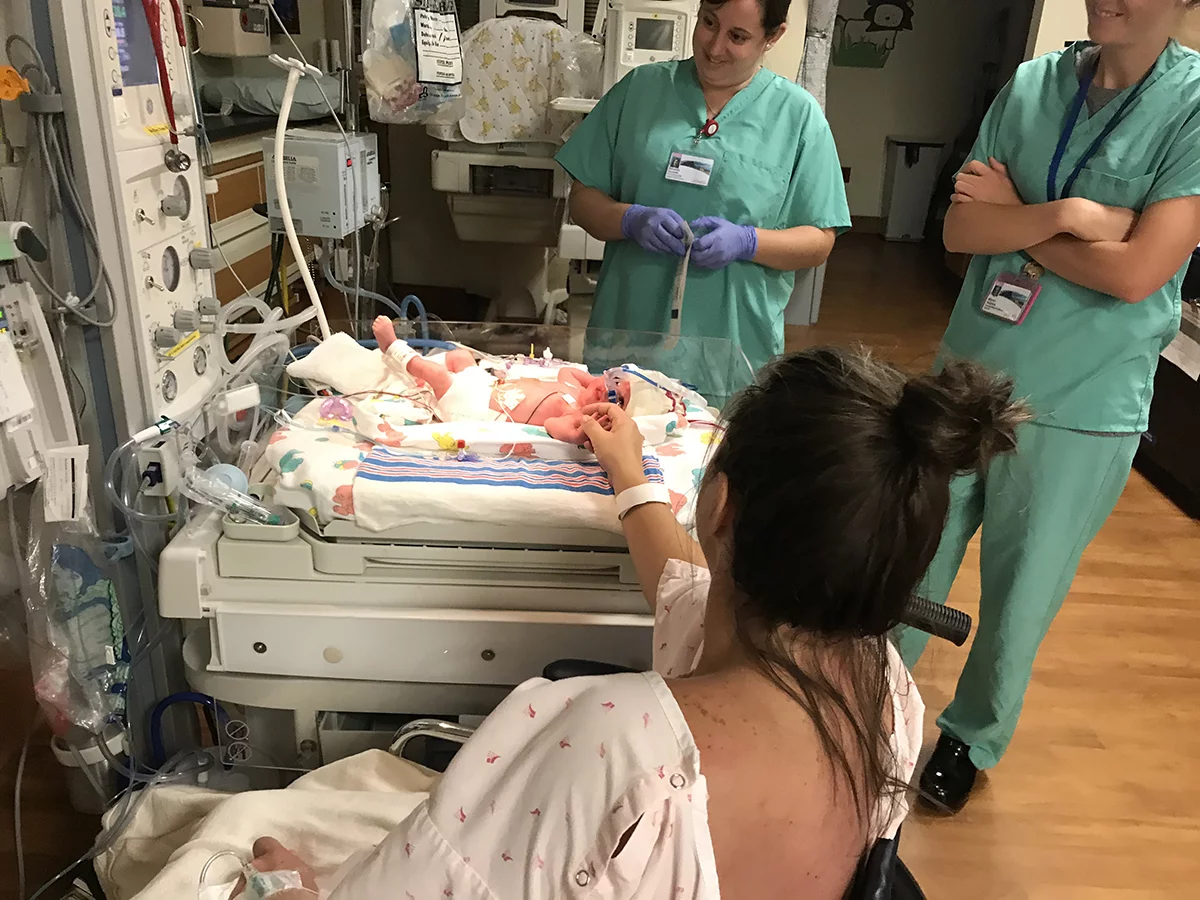
“Graham had prepared me about what she was going to look like, with tubes and cords everywhere,” said Erin. “When we went together for the first time, we were a family, even though the circumstances were dire. Mom and baby were there.”
Erin turned on her “strong mama bear brain,” feeling the need to be strong for both Graham and their daughter.
“I needed to tell myself it was going to be ok,” she said. “I told her, ‘I’m your mom and it’s going to be ok.’ I said the words even though I didn’t know if it would be true.”
More positives than negatives
Forty-eight hours after she was born, Erin was able to hold her daughter skin-to-skin.
“If you moved her wrong, it felt like you would have pulled out one of her lifelines,” she said. “There were wires from her umbilical cord, leads on her chest, a CPAP mask to help her breathe, the feeding tube.”
“She was so small, you could have picked her up with chopsticks,” said Graham.
With every hour and day that ticked by, Erin and Graham looked for silver linings.
“When the CPAP mask came off and she moved to high-flow oxygen, it was a step forward,” said Erin. “That let us know her lungs were developing more which was her main struggle. We were making preemie steps.”
Three steps forward, two steps back – the “NICU dance.”
As Erin’s milk began to come in, she had a new focus.

“Pump, eat, sleep. Pump, hold, sing. Every three hours, I pumped like it was my job,” she said. “She had to eat every three hours, and that was something I was able to do that would help heal her and make her stronger. It gave me hope and a purpose.”
After nearly a week, Erin and Graham decided on a name – Mimi Elaine McDaniel.
“She’s named after my grandmother, who for most of her life had lymphoma,” said Graham. “She was a fighter and was always happy even when she was struggling. Mimi was showing us that resiliency, too.”
Finding strength and support in a new “family”
Mimi grew stronger with each day in the special care nursery. The strength of Erin and Graham’s marriage was also evident.
“We leaned on each other more during the time Mimi was in the hospital than we ever have,” said Erin. “In our 15 years together, this is the hardest thing we’ve ever experienced.”
“Our baby’s life was on the line, and we had a toddler at home who still needed her mom and dad in her life,” said Graham.

Mimi being able to stay in the special care nursery at YVMC, with the oversight of local pediatricians and the neonatal nurse practitioners from Children’s Hospital Colorado, allowed Eddy’s everyday routine to remain largely in place. Graham was able to pick her up from preschool during the week and bring her to the hospital to see where Mimi was “living in the hospital with the doctors,” as Eddy described it.
“It could have been so much harder on Eddy if we had to be in Denver,” said Erin. “It really helped us heal emotionally and get through those weeks to have access to our home and our pillows.”
Getting to know the nurses and neonatal practitioners over the weeks provided comfort, too.
“Being there for so long, we knew all their names, their kids’ names, what kind of pets they had. They become an extension of your family,” said Erin. “I knew it was ok to run home quick because Faith had her, or she’s with Melissa right now, or Ellen’s on tonight so I know I can get a shower.”
Home at last

On Oct. 9, just seven days short of her original due date, Erin and Graham brought Mimi home.
“Mimi went from needing so much help from the doctors and nurses at the hospital just to live, to being home with us as a family,” said Erin. “I had to wait four weeks for the Instagram photos I had envisioned on our bed with my daughters, but it felt so good to finally be home together.”
