Their story begins in North Palm Beach, Florida, in August 1964. Their first encounter was anything but pleasant.
That week, David Harvey and Sharon Jordan met over a game of Scrabble and when David won, he acted like a brat, reveling in victory like a prize fighter after winning the big one. David told her he would love to beat her again sometime. Sharon told her mother that if she never saw him again, so be it. He was pompous and conceited.
At Christmas that year, David, who lived in Gainesville, Florida, was in North Palm Beach for a week-long conference. Sharon, a third-grade teacher, was sitting on the beach looking out over the water. David picked up two cans of soft drinks and walked over and stood beside and a little behind her. After a minute or so, she saw him out of the corner of her eye and said “Hi.” He said: “I just happen to have two pops here and can drink only one. Would you like one?’’

It was a terrible, hokey pick-up line that started their 51-year relationship. They saw each other every day for five days before David returned to his home in Gainesville. Smitten with each other, they wrote letters, talked on the phone, and David made the 560-mile round trip every other week.
By mid-January, they were talking about marriage. On Dec. 18, 1965, they exchanged vows to stay together in sickness and in health. They were true to their pledge, though in the end, despite the best effort of the couple and others, their life together was cut short by the unexpected.
Their bond lasted decades, bringing them two daughters – Lynda and Rena – three grandchildren and a host of friends. After their early years together in Boca Raton, Florida, they moved to western Pennsylvania, then to southern Colorado to retire and to be near their daughters.
In April 2015 they had a fortuitous encounter at a neighborhood party with Jerry and Carla Bowen. Carla, it turned out, was the director of Primary Care for Colorado Health Medical Group in Colorado Springs. If David and Sharon ever needed a good doctor, Carla said, she knew a bunch of them.
Two months later, the couple called on Carla after a routine colonoscopy showed Sharon, 74, had a cancerous tumor in her colon. “Sharon was thinking, ‘Rats! I have gotten through my whole life to this point without needing surgery of any sort,’’’ David said.
Carla recommended that the Harveys schedule an appointment with Dr. Tiffany Willard, a general surgeon with CHMG at Memorial and a team that included oncology and gastroenterology specialists.
“Dr. Willard got us focused on what probable treatment procedures and sequences would be, and she explained that there were several different imaging procedures that needed to be done before chemo/radiation and the first surgery,’’ David said.

Sharon committed to fighting the disease. Imaging established the size and nature of the tumor. Sharon’s team prescribed five weeks of radiation and chemotherapy, with surgery to follow. They answered every question about the treatments, David said. He also saw their professionalism.
“I was impressed to see how the team worked and how everyone on the team [physicians, nurses, and staff personnel] were working together and pulling for her. They were determined to do what they could to make it happen,’’ he said.
Before radiation therapy, a custom plastic form – one that would help keep her still while the radiation was delivered – had to be made so the radiation could be focused precisely on the tumor. Chemotherapy was delivered through an IV.
By the end of radiation and chemo, the active and aggressive tumor had shrunk to no more than an ulcerated spot on the wall of the colon and there were no signs of cancer in the colon.
The Harveys were again impressed with the coordination of care – infusion room nurses working alongside pharmacists who assembled the chemotherapy before Sharon received it.
“Sharon saw how much they all cared, how they nurtured her through the processes, and she was massively encouraged. Sharon very much appreciated the kind of care that the radiation and chemo nurses and staff provided,’’ David said.
When she went home to rest, Sharon found particular comfort in reading to the grandkids and spending time with them. They helped sustain her, along with her daughters Lynda and Rena.
Following the therapy, Sharon rested for a month, healed and gained strength before surgery on Oct. 19, 2015. That day, Dr. Willard removed 8 or 9 inches of the colon and established an ostomy, a surgical opening in the body for the discharge of bodily waste. The surgery went very well.
At a care conference after the surgery, when more than 40 people — doctors, nurses, and techs – packed a room, there was more good news.
“Dr. Willard presented details about Sharon, including the report on biopsies of 23 lymph nodes in which every single biopsy was negative. Dr. Willard said that doesn’t often happen and the case got applause from peers,” David said.
Sharon went home three days after the first surgery. She was encouraged. She was told to rest for a month. She needed it. The chemotherapy (24/7 for over four weeks) and radiation (5 days a week for 5 weeks) had been grueling and she was ready for a break.
Through late November, doctors began talking to Sharon about another surgery – one that would reverse the ostomy and reconnect the smaller and larger intestines. After some discussion, Sharon decided on two phases of chemotherapy to prepare for surgery. David and Sharon celebrated the beginning of the second phase on Dec. 1, 2015 and 50 years of marriage on December 18. Sharon completed the chemo on March 10, 2016, writing “YEA!” on the calendar in celebration.
Sharon had the ostomy reversal surgery April 21, 2016 and Dr. Willard told David afterwards that she was pleased with how well Sharon was doing.
“Everything had gone great. Sharon thought she would be in for a day or two – perhaps go home on Saturday or Sunday. She was very excited about her prospects at that point,’’ David said.
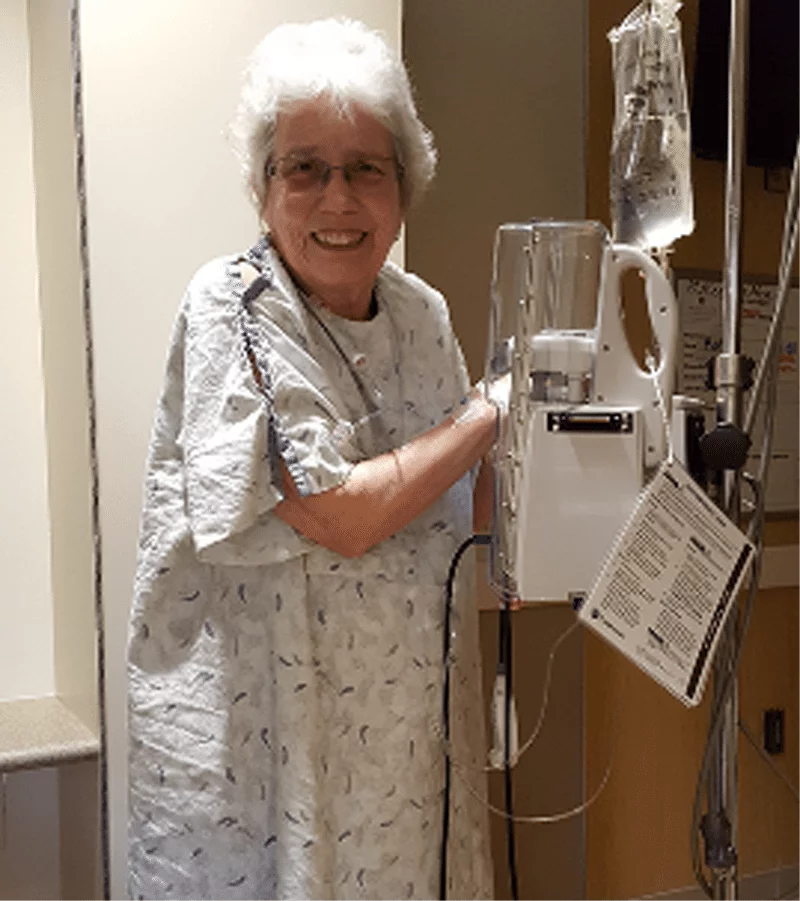
On Friday, Sharon got out of bed and walked in the hallways pushing her IV pole along with her. Someone snapped a photograph showing her walking and smiling. On Saturday, she had another great day. Her sister-in-law, Liz, was with her for several hours and they had an uproariously good time. Liz said that Sharon was in as good a mood as she could remember.
Nurses checked on Sharon regularly post-surgery. They monitored vital signs to make sure she was okay.
“She was just as happy as she could be. One of the nurses left the room after checking on her – there was no reason not to – and when she returned 15 minutes later, Sharon was unresponsive, gone,’’ David said.
She died from a pulmonary embolism, a blockage of an artery in the lungs by a substance that traveled from elsewhere in the body. It is one in a laundry list of side effects that can happen during or after surgery.
“It is recognition that no matter how high-tech the process is, or how expert the personnel are, no human is exempt from the influences of the unknown and uncontrollable,’’ David said.
David got the call from a nurse when he was shopping with his daughter, Lynda, at City Market in Cañon City. He and Lynda drove to Memorial Hospital. On the ride, he tried to come to grips with the fact that the woman he had met on the beach so many years ago had passed. He reflected on how she cared for her students, including a third grader who once told her: “Is too bad you ain’t got no kids. You is so loving.’’ He remembered how the student recognized the love and care that Sharon directed towards her and all the parents and students who spoke over the years of her loving nature.
Before David and Lynda got to the hospital, Dr. Willard stopped by and was visibly upset about Sharon’s unanticipated death. She commented that “this was heartbreaking,” David said.
Nurses and others offered their heartfelt condolences.
“I appreciated their offerings and I’m thankful for their service to Sharon and our family. The compassion that all of them displayed over losing Sharon was, for the family members, a needed uplifting gift in the face of loss,’’ David said.